We could know soon whether vaccines work against a scary new coronavirus variant
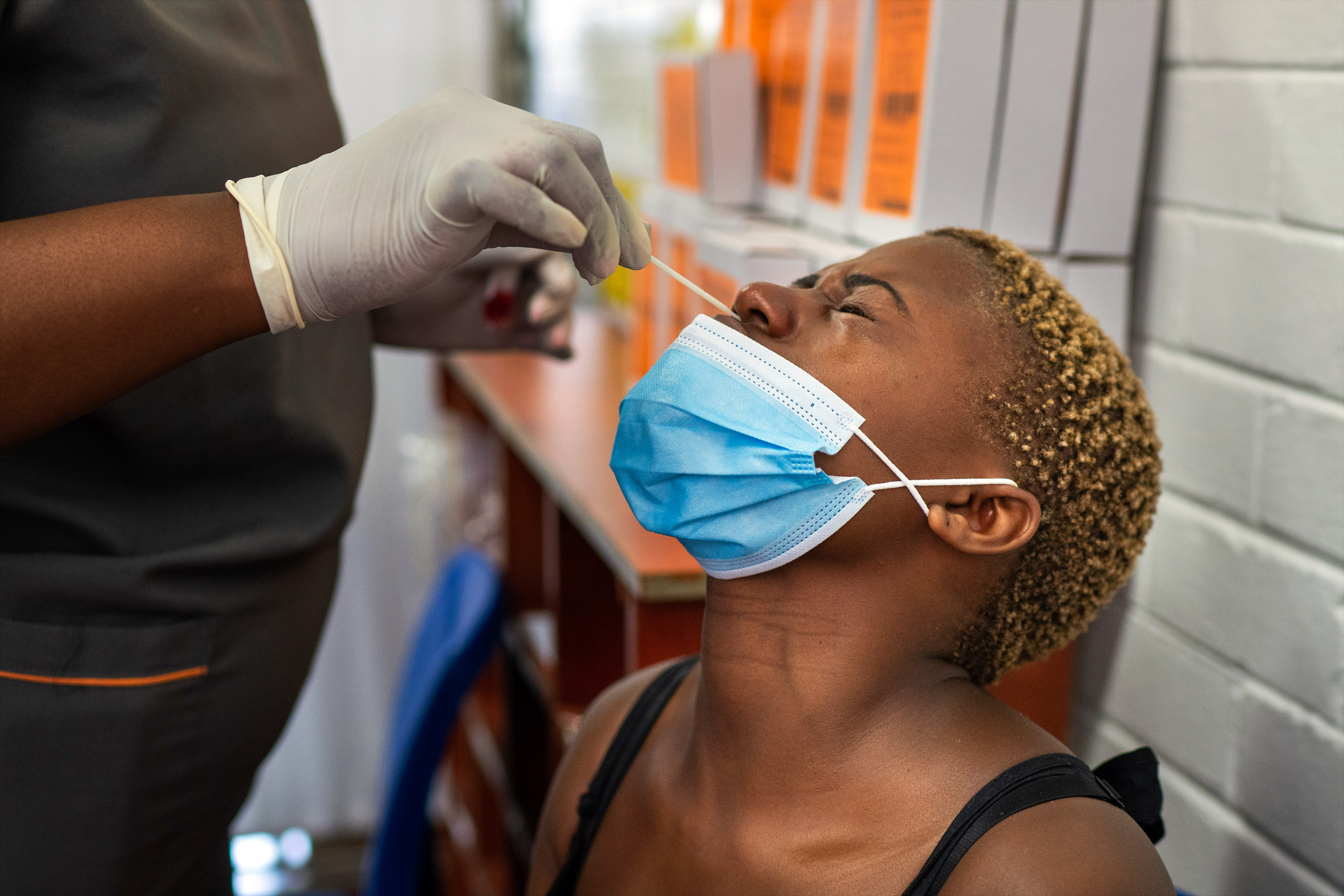
Salim Abdool Karim was at a cricket match on December 26, Boxing Day, when he made the mistake of looking at his email. He had received a new report and the news wasn’t good. A heavily mutated coronavirus spotted in South Africa appeared to allow the virus to bind more tightly, and more easily, to human cells.
Karim, an epidemiologist and lead covid-19 adviser to the South African government, knew what the report meant. It could explain a drastic change in covid-19 in his country, where rising case numbers were turning every province red.
“It simply went up, up, up, and up, into the equivalent of an Everest,” Karim says.
The rise in cases in South Africa has been linked to a new, highly mutated form of the covid-19 virus. And it's just part of a wider pattern being seen around the world. Over the last month, weary researchers racing to understand new variants in Africa, Brazil, and the United Kingdom have pumped out a series of alarming reports on preprint servers, websites, and in official reports, describing a coronavirus that is changing in ways that appear to let it shrug off lockdowns, avoid antibodies, and retake cities, like London or Manaus, that already suffered through big first waves.
Indeed, in a few short weeks the perception among some scientists of the coronavirus has gone from a static, slow-changing virus that’s easily walloped by vaccine technology to something more like a terrorist shapeshifter that could put a decisive end to the pandemic out of sight.
Will vaccines still work?
Most the world’s attention has been on a so-called British variant of the covid virus; it seems to spread faster than the original version and has appeared in dozens of countries, including the US. On Friday, January 22, the UK prime minister, Boris Johnson, said government advisers warned this strain may also be more deadly, killing the infected about 30% more often.
Faster spreading, more deadly, versions of the coronavirus can still be dealt with using masks and social distancing. But the variant in South Africa, called 501Y.V2 and first described by gene sleuths on December 22, not only spreads faster but, alarmingly, also appears to evade antibodies from the blood of people previously infected by covid-19, and, in theory, could also lessen the effect of vaccines, society’s main hope of curbing the global outbreak.
Such lab evidence of “immune escape” makes the variant in South Africa “much more concerning” than the one in the UK, according to Anthony Fauci, director of the US National Institute of Allergy and Infectious Diseases, speaking at his first press conference under the new Biden administration on January 21. “The real question that people are quite clearly interested in is: What is the impact on the vaccine?” Fauci said.
What Fauci didn’t mention is that we could have a real-world answer to that question as soon as next week thanks to a large vaccine trial that recruited thousands of South Africans between September and December, just as the dangerous variant spread widely.
That vaccine, from Johnson and Johnson, has been widely anticipated because it’s given as single shot and is easily stored, making it easier to get into arms than the super-cooled, two-dose messenger RNA vaccines from Moderna and Pfizer authorized in the US last month.
Now, though, the J&J trial may unexpectedly answer the big question of whether vaccines will protect against the 501Y.V2 variant in South Africa or not. That could be determined if data show the shot is less effective in South Africa than it has been in the US, where part of the trial occurred.
“It will be wonderful if it has equal efficacy against the South Africa strain. If it doesn’t, that is telling us something,” says Lawrence Corey, a virologist at Fred Hutchinson Cancer Research Center in Seattle, who leads the operations center for the COVID-19 Prevention Network, which coordinates vaccine trials financed by the US government.
Corey estimates that 7,000 South Africans joined the trial, and since it took place as the new virus spread, “most of the study in South Africa will be measuring the efficacy against the variant.”
Second waves
The worry is that all major vaccines were constructed using the genetic information that became available on the virus a year ago. And since then, the virus has kept changing. If the vaccines aren’t as effective against new strains, that, in turn, would make it harder to “crush the curve” of cases, hospitalizations, and deaths.
During scientific presentations broadcast on January 18, Karim described how every province in South Africa saw a dramatic rise in cases during December. “This drastic change that we are seeing is being driven by a virus that certainly looks, biologically, that it can attach to human cells more efficiently,” he says. “Our second wave reached completely new heights, we are now seeing, today, more cases and more deaths than we ever, on any day, saw in the first wave.”
When it was first detected, the South African variant looked worrisome because of the large number of mutations it had gained, 23 in all, and how many of these were in the critical spike protein, which the virus uses to attach to human cells. That strongly suggested the virus was evolving to avoid antibodies.
Since then, researchers have gathered more alarming clues about 501Y.V2, including from a study that showed that antibodies in blood serum from around 50 people previously infected were frequently unable to block the new variant.
“When you test the blood from people in the first wave [we find] in nearly half the cases there is no recognition of the new variant,” Penny Moore, a researcher at the University of the Witwatersrand in Johannesburg, said during the same broadcast.
That’s concerning, but vaccinations may elicit a broader, more powerful immunity than a passing infection, so it’s impossible to say they won’t still work. And Moore said that blood from some patients, especially those who’d become very sick, were still able to neutralize the variant, at least in lab tests. “That is important when we think of vaccine, some vaccines elicit very high level of antibodies and others do not,” she said.
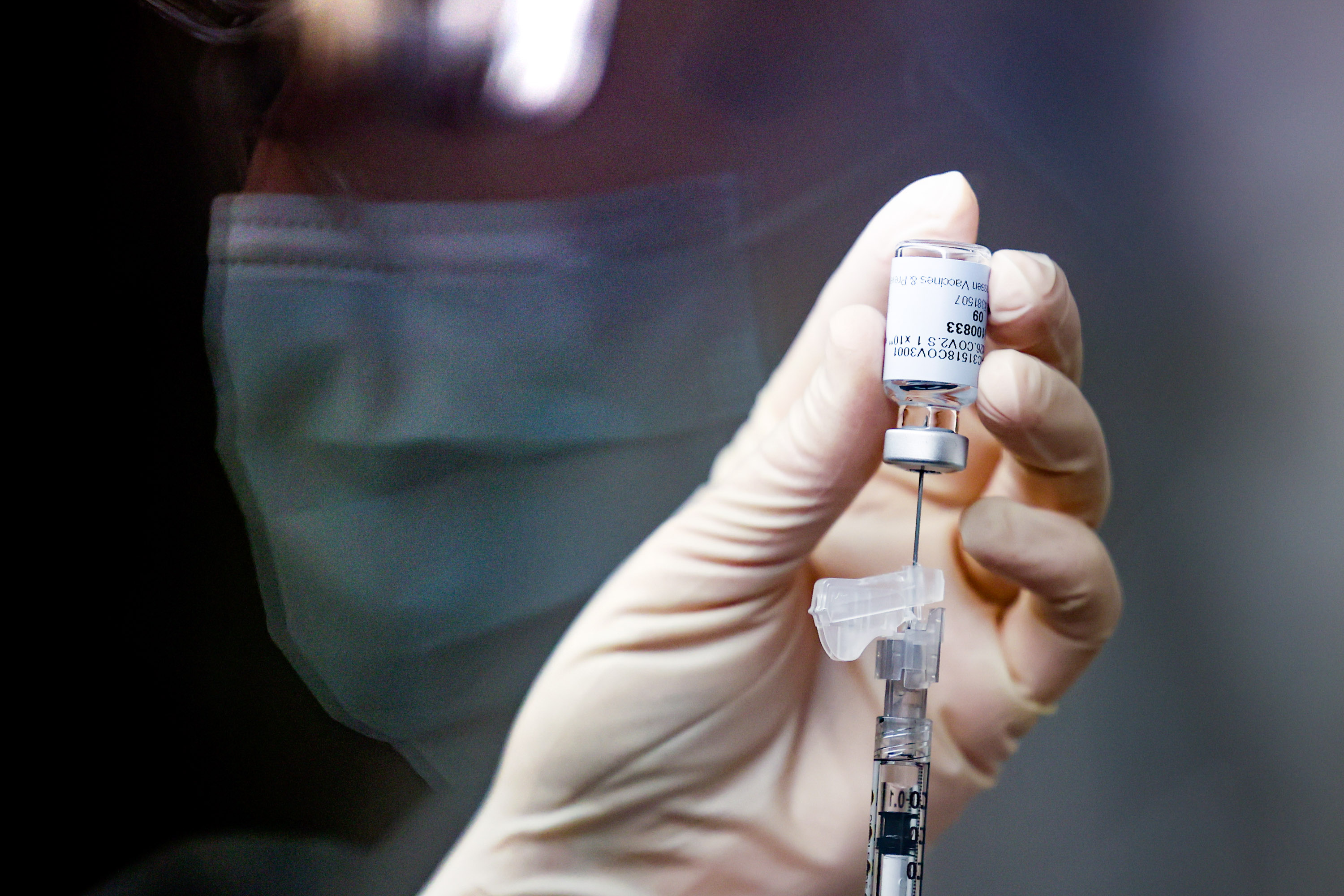
Another signal in favor of vaccines is that, so far, there is no clear evidence that the new strain is more likely to re-infect people who’ve had covid-19 before. If natural immunity does in fact hold up, then immunity gained from a vaccine likely would as well. “Are we seeing a systematic increase in reinfection? The data don’t allow us to say,” Karim says. Reinfection could still be prevented, he says, because the body “has two immune mechanisms, B cells that make antibodies, and T cells that go around gobbling things up and killing them.”
Researchers say that laboratory tests alone can’t prove whether vaccines will work against the new variants, and why they hope results from actual ongoing trials of vaccines in South Africa, the UK, and elsewhere may soon give better answers. “We are expecting an answer pretty soon," Karim says. “But we want to see the actual data, and it is not yet available.”
Convergent evolution
Scientists are looking at two major possibilities where these variants are coming from. One hypothesis is the virus is evolving inside immune-compromised people, where it can persist for months while learning to dodge the immune system. Another idea is that variations are arising in cities like London, which suffered big infection waves early in 2020. Millions were infected, but if their antibodies waned over the year, then their bodies could be selecting for virus variants able to resist what remains of their immune response.
Some scientists now think that evolved variants are probably cropping up everywhere, not just in Britain and South Africa, but just haven’t been detected yet. “We expect as people increase genomic surveillance, multiple variants will be discovered, especially in places that have had a lot of cases for a long time,” says Tulio de Oliveira, who studies viral genomes at the University of Washington. “Unless we can suppress transmission to almost zero, the virus will keep outsmarting us.”
Scientists say they are fairly sure the variants in South Africa and the UK spread faster, causing about 50% more follow-on infections than the original strain from China. Part of the evidence is how fast the UK variant, called B.1.1.7, has taken hold elsewhere, outcompeting older versions. It already accounts for nearly half of cases in Israel, which is facing a peak in infections despite a big vaccination campaign. The 501Y.V2 variant, meanwhile, has already been seen in at least 10 countries.
Some of these variants share mutations, including one called N501Y, the one that lets it bind more tightly with human cells. To scientists, the copycat mutations arising in different continents means the virus is undergoing “convergent evolution.” That is, different variants of the virus are hitting upon the same strategies to escape the pressure of antibodies in the blood of those infected or vaccinated.
Waiting for answers
The big Johnson and Johnson study launched in September and finished enrolling 45,000 participants on December 17, according to the company, which says it will learn if the vaccine is effective by the end of January. If the results are positive, it could apply for authorization soon after.
Academic and government scientists, along with Johnson and Johnson, decided on an international approach for that vaccine and trialed the shot in Africa, Brazil, and other parts of Latin America, as well as the US. Now that move looks prescient. Their study launched exactly when the new variant was taking hold in South Africa. And it soon took over: more than 80% of cases in South Africa are now being caused by the variant.
“We wanted it to be globally relevant,” says Corey. “We hadn’t appreciated that strain variation would occur so quickly, but it’s allowing us to get an early read on what is happening and that is very fortunate.” A spokesperson for Johnson and Johnson said the company could not comment on the trial results until they become public. The company did not confirm how many South African volunteers were part of the study.
Researchers have started to plan how they could alter, or update, the vaccine shots to deal with new strains. The two messenger RNA vaccines can be reprogrammed fairly easily, according to the companies making them. That’s likely also the case with the Johnson and Johnson vaccine, which employs a harmless type of cold virus, to which a section of coronavirus is added.
To deal with variants, Corey says, it’s also possible the doses could be increased or boosted later on with “strain-specific” follow-up shots. Another idea is to aim vaccines at different parts of the virus that are slower to evolve than its spike protein, but such vaccines would take longer to develop and test.
Researchers in South Africa emphasized they can’t yet say that existing vaccines won’t work against the variant in their country, and several said they would definitely take a vaccine if it was offered. What they do believe is that the world has underestimated the virus, which is continuing to adapt and evolve.
Deep Dive
Biotechnology and health
How scientists traced a mysterious covid case back to six toilets
When wastewater surveillance turns into a hunt for a single infected individual, the ethics get tricky.
An AI-driven “factory of drugs” claims to have hit a big milestone
Insilico is part of a wave of companies betting on AI as the "next amazing revolution" in biology
The quest to legitimize longevity medicine
Longevity clinics offer a mix of services that largely cater to the wealthy. Now there’s a push to establish their work as a credible medical field.
There is a new most expensive drug in the world. Price tag: $4.25 million
But will the latest gene therapy suffer the curse of the costliest drug?
Stay connected
Get the latest updates from
MIT Technology Review
Discover special offers, top stories, upcoming events, and more.