Covid-19 vaccines shouldn’t get emergency-use authorization
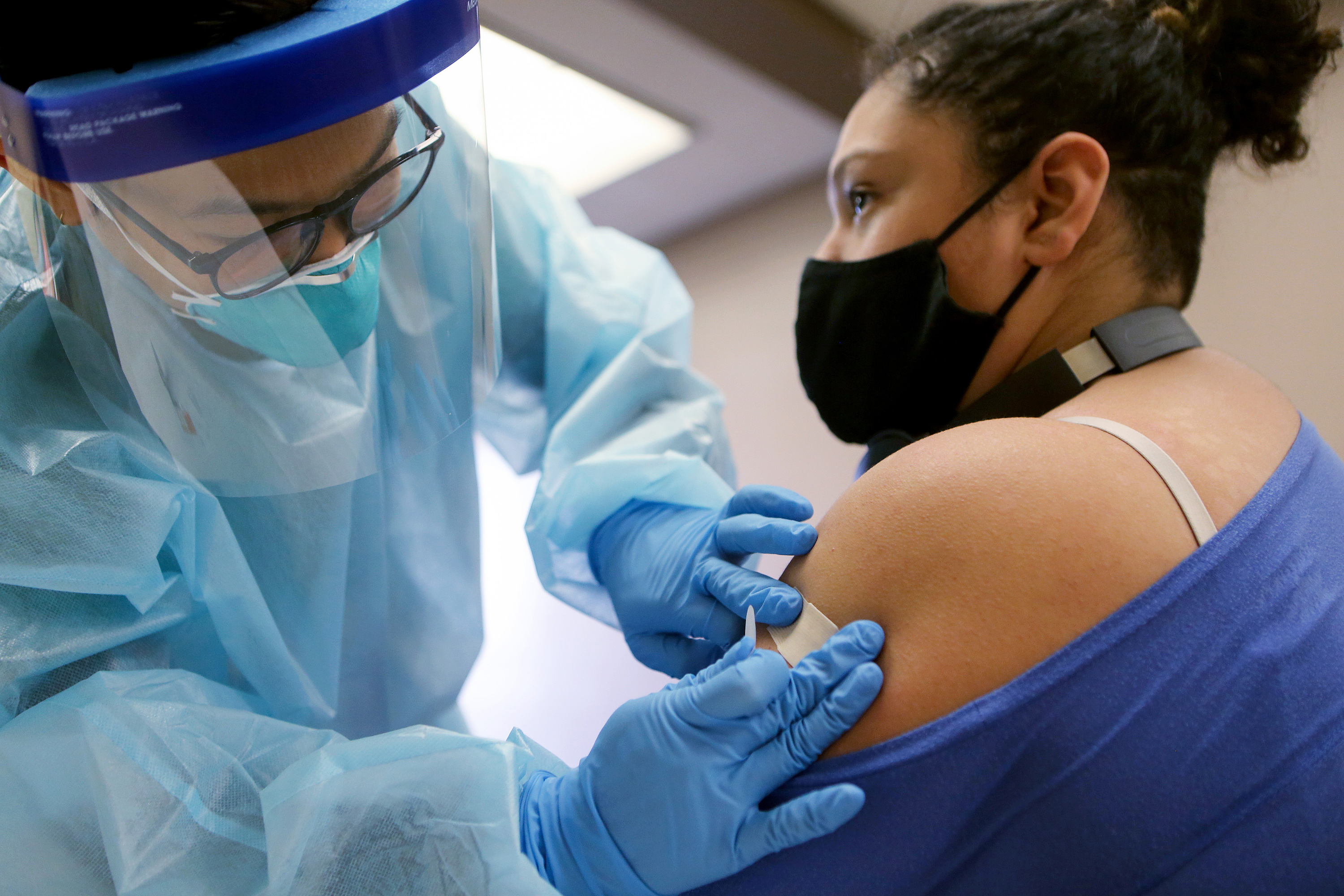
I really want a covid-19 vaccine. Like many Americans, I have family members and neighbors who have been sickened and killed by the new coronavirus. My sister is a nurse on a covid-19 ward, and I want her to be able to do her job safely. As a health-care lawyer, I have the utmost confidence in the career scientists at the US Food and Drug Administration who would ultimately determine whether to issue an emergency-use authorization for a covid-19 vaccine. But I am deeply worried about what could happen if they do.
The pace of covid-19 vaccine research has been astonishing: there are more than 200 vaccine candidates in some stage of development, including several that are already in phase 3 clinical trials, mere months after covid-19 became a global public health emergency. In order for the FDA to approve a vaccine, however, not only do these clinical trials need to be completed—a process that typically involves following tens of thousands of participants for at least six months—but the agency also needs to inspect production facilities, review detailed manufacturing plans and data about the product’s stability, and pore over reams of trial data. This review can easily take a year or more.
That’s why, for several months now, the FDA has been considering criteria for initially deploying a covid-19 vaccine under an emergency-use authorization, or EUA, before the FDA has all the information normally required for full approval. At least a few of the manufacturers currently in phase 3 trials have publicly stated their intent to request an EUA. Pfizer plans to do so later this month in light of the exciting preliminary results for its vaccine.
EUAs allow the FDA to make unapproved products available during public health emergencies. While the FDA has issued EUAs sparingly for diagnostics and therapies aimed at other infectious diseases, such as H1N1 and Zika, a vaccine has never been used in civilians under an EUA. Vaccines are different from other medical products in that they are deployed broadly and in healthy people, so the bar for approving one is high.
The FDA’s Vaccines and Related Biological Products Advisory Committee, a group of outside experts who advise the FDA on vaccines, met for the first time to discuss covid-19 vaccines on October 22. Some committee members questioned whether the FDA had set the bar for a vaccine EUA high enough. Members also expressed several important concerns about authorizing a vaccine through an EUA.
One concern is that once a vaccine is authorized in this manner, it may be difficult—for ethical and practical reasons—to complete clinical trials involving that vaccine (and thus to collect additional safety data and population-specific data for groups disproportionately affected by covid-19). It could also hamper scientists’ ability to study other covid-19 vaccine candidates that may be “better” in various ways than the first across the finish line.
But the most important consideration in my view relates to public trust.
Public health experts caution that vaccines don’t protect people; only vaccinations do. A vaccine that hasn’t gained enough public trust will therefore have a limited ability to control the pandemic even if it’s highly effective.
Data from the Pew Research Center show declining trust in a covid-19 vaccine across all genders, racial and ethnic categories, ages, and education levels, with many people citing safety and the pace of approval as key factors in their skepticism. Information presented to the advisory committee by the Reagan-Udall Foundation similarly showed significant distrust in the speed of vaccine development, likely exacerbated by recent political interference with the FDA and the US Centers for Disease Control and Prevention (CDC) and some politicians’ promises that a vaccine would be available before the end of the year. People of color have expressed additional concerns with vaccine research.
Judging from their written and verbal comments to the advisory committee, major vaccine manufacturers recognize the potential disruptions to subsequent clinical trials and are seeking the FDA’s advice to address them. While those considerations are daunting, I suspect that manufacturers and the FDA could create workable responses. But even then, the public trust issues associated with EUAs—which most of the public first heard about through the hydroxychloroquine debacle and again in the context of the convalescent plasma controversy—still make this tool a poor fit for vaccines.
Instead, if vaccine trial data are promising enough to warrant giving some people pre-approval access to a covid-19 vaccine, the FDA should do so using a mechanism called “expanded access.” While the FDA ordinarily uses expanded access to make experimental treatments available to sick patients who have no alternative treatment available, it has been used for vaccines before and could be used now to avoid disrupting ongoing clinical trials or fostering public perceptions that a vaccine was being rushed because of an “emergency.” Expanded-access programs are also overseen by ethics committees and have informed consent requirements for patients that go beyond those associated with products authorized by EUA.
Not only must the public trust a covid-19 vaccine enough to seek out the first wave of authorized vaccines, but that trust must be resilient enough to withstand potential setbacks: protection below 100% (and perhaps below 50%), significant side effects (or rumors of them), and possible recalls. That level of trust takes time to rebuild if it has been eroded. And the stakes here are not just the slowing of this pandemic. As former senior health official Andy Slavitt recently said, “Done right, vaccines end pandemics. Done wrong, pandemics end vaccines.”
Clint Hermes, a former academic medical center general counsel, has advised universities, teaching hospitals, and life sciences companies on global health problems. He has helped set up vaccination, treatment, and surveillance projects for infectious diseases in North and South America, Africa, Asia, and the Middle East. The views expressed here are his own and not those of any organization with which he is affiliated, including his employer. The information presented here should not be construed as legal advice.
Deep Dive
Biotechnology and health
How scientists traced a mysterious covid case back to six toilets
When wastewater surveillance turns into a hunt for a single infected individual, the ethics get tricky.
An AI-driven “factory of drugs” claims to have hit a big milestone
Insilico is part of a wave of companies betting on AI as the "next amazing revolution" in biology
The quest to legitimize longevity medicine
Longevity clinics offer a mix of services that largely cater to the wealthy. Now there’s a push to establish their work as a credible medical field.
There is a new most expensive drug in the world. Price tag: $4.25 million
But will the latest gene therapy suffer the curse of the costliest drug?
Stay connected
Get the latest updates from
MIT Technology Review
Discover special offers, top stories, upcoming events, and more.