Merck’s Vaccine Won’t Be the End of Ebola
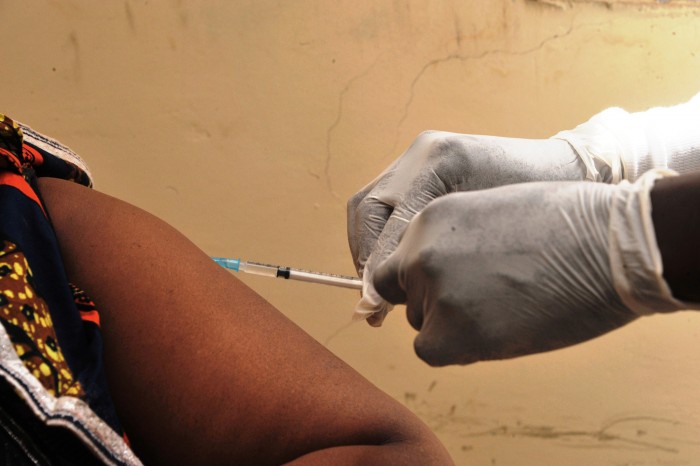
An Ebola vaccine that has been in development for 15 years has been shown in a clinical trial to be up to 100 percent effective at preventing the deadly virus. But it won’t stop sporadic cases from popping up, nor will it be immediately available to some who are most vulnerable to the virus.
Marie-Pierre Preziosi, medical officer of the Initiative for Vaccine Research at the World Health Organization, which led the trial, says the vaccine is only meant to be used to stop the spread of an emerging outbreak. Once WHO identifies new Ebola cases, only people most at risk of being exposed to a sick person—like family members, health-care providers, or sanitation workers—would receive the vaccine if it’s approved.
Preziosi says the vaccine won’t be administered as a preventive vaccine on a large scale, like vaccine campaigns for smallpox or polio, because there’s not enough data to show how long the vaccine’s protection lasts and because it only targets one strain of the virus. If the vaccine is approved by drug regulators, it wouldn’t be used for a “long-term strategy” to thwart new Ebola cases, she says.
This approach is similar to oral cholera vaccines, which are used during outbreak situations or before travel to an area prone to cholera. Despite the availability of these vaccines, cholera outbreaks still occur throughout the developing world. Many vaccines are believed to provide several years to decades of protection against disease.
Nearly 12,000 people in Guinea were involved in the trial, which began in 2015 after the Ebola outbreak was in full swing. Among the nearly 6,000 people who received the vaccine, no Ebola cases were identified 10 days or more after vaccination. In those who did not receive the vaccine, 23 cases appeared within the same time frame.
Manufactured by Merck, the vaccine uses a genetically engineered version of vesicular stomatitis virus, an animal virus that primarily affects cattle, to carry an Ebola virus gene insert. The final results of the trial were published at the end of last month in the Lancet.
Jesse Goodman, founding director of Georgetown University’s Center on Medical Product Access, Safety and Stewardship, says the study results are “impressive” but there are still many unknowns about the vaccine, including its effectiveness and whether it will be safe for pregnant women, HIV-positive individuals, and young children. Goodman is on the board of directors at GlaxoSmithKline, which is also developing an Ebola vaccine in partnership with the National Institutes of Health.
Studies in HIV-positive individuals and children younger than six are just getting started, says Tom Monath, chief scientific officer and chief operations officer at NewLink Genetics, which initially licensed the vaccine from Canadian government scientists and is collaborating with Merck.
Scientists will be able to glean only limited information from these additional studies, though. Now that the Ebola outbreak has ended, researchers will not be able to measure the vaccine’s efficacy in these subjects. They can’t expose trial volunteers to Ebola since the virus is so deadly.
Preziosi says a combination of Ebola therapeutics and vaccines, including one that could protect against different strains of the disease, will be needed in order to effectively prevent and respond to future outbreaks.
Keep Reading
Most Popular
How scientists traced a mysterious covid case back to six toilets
When wastewater surveillance turns into a hunt for a single infected individual, the ethics get tricky.
The problem with plug-in hybrids? Their drivers.
Plug-in hybrids are often sold as a transition to EVs, but new data from Europe shows we’re still underestimating the emissions they produce.
What’s next for generative video
OpenAI's Sora has raised the bar for AI moviemaking. Here are four things to bear in mind as we wrap our heads around what's coming.
Stay connected
Get the latest updates from
MIT Technology Review
Discover special offers, top stories, upcoming events, and more.