Tiny Brain Clumps Offer New Clues into the Cause of Autism
By turning stem cells taken from autistic patients into tiny “organoids” that closely resemble the brains of human embryos, researchers have gleaned potentially valuable insights into what may go wrong during brain development in people with autism.
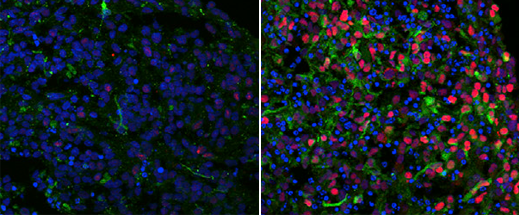
The work, published today, illustrates the value of using three-dimensional brain structures, which re-create natural conditions more accurately than traditional two-dimensional cell cultures, to investigate the physical basis of poorly understood brain disorders. Though some 80 percent of autism cases have no clear genetic cause, it is generally accepted that the disorder can be traced back to things that go wrong during early brain development, and the ability to observe embryonic brain development could yield valuable insights that may reveal how to treat or even reverse it. Other researchers are now investigating the potential of using organoids to study other misunderstood diseases like schizophrenia and Alzheimer’s (see “10 Breakthrough Technologies 2015: Brain Organoids”).
Much of the investigation into the causes of autism has focused on searching through patients’ genomes for mutations and then using animal models to study the roles the affected genes play in brain development. This is the first published study using brain organoids to investigate the disorder. The researchers identified commonalities among organoids made from the cells of these patients and worked to determine their genetic basis.
Led by Flora Vaccarino, a professor of child psychiatry and neurobiology at Yale University, the researchers began by selecting autistic patients with enlarged heads, a condition that affects about a fifth of people with the disorder. They took skin cells from four patients and turned them into stem cells capable of developing into many kinds of specialized cells. Then they directed those cells to develop into the types of neurons found in the forebrain. For comparison, they did the same using cells isolated from the patients’ fathers, who did not have autism.
After growing the organoids, the researchers performed a variety of different analyses, including genetic sequencing and physiological tests, to confirm that the structures reproduced various important components present in the brain of a developing fetus. Then they compared the organoids made from the patients’ cells with ones made from the cells of their fathers, identifying certain genes that were expressed differently. In particular, they noticed that genes involved with directing the proliferation of cells were overexpressed in the autistic organoids. Further analysis revealed a disproportionate number of a certain type of neuron compared with another type that is normally present in roughly the same number.
Finally, they looked back at the gene expression data and found that the autistic organoids had much more expression of one particular gene that is important in early brain development. When the researchers engineered the DNA to reduce the expression of that gene, they were able to turn cells from the autistic patients into organoids without the neuronal imbalance they saw before.
The results provide potential routes to targeted therapies, demonstrating the power of an approach that is quickly gaining momentum within the research community, says Madeline Lancaster, a group leader at the Medical Research Council’s Laboratory for Molecular Biology in the United Kingdom. Lancaster helped develop a slightly different method for making organoids and has used them to study microcephaly, a rare neurodevelopmental disorder that leads to abnormally small head size. That research was the first demonstration of organoids as models for a neurological disorder.
Lancaster and others are now hoping to study more common diseases this way. The new work is encouraging, she says, because it confirms that organoids can be used to study autism, a “more subtle” neurological disease than microcephaly. It hadn’t been clear whether it would be possible to perceive such subtlety in an organoid.
Keep Reading
Most Popular
How scientists traced a mysterious covid case back to six toilets
When wastewater surveillance turns into a hunt for a single infected individual, the ethics get tricky.
The problem with plug-in hybrids? Their drivers.
Plug-in hybrids are often sold as a transition to EVs, but new data from Europe shows we’re still underestimating the emissions they produce.
What’s next for generative video
OpenAI's Sora has raised the bar for AI moviemaking. Here are four things to bear in mind as we wrap our heads around what's coming.
Stay connected
Get the latest updates from
MIT Technology Review
Discover special offers, top stories, upcoming events, and more.