Is a covid and flu “twindemic” on the horizon?
Covid cases may be rising just as we enter flu season in the Northern Hemisphere.
This article is from The Checkup, MIT Technology Review's weekly biotech newsletter. To receive it in your inbox every Thursday, sign up here.
Hello, and welcome back to The Checkup!
I’m back home in London after last week’s trip to the Swiss Alps to meet millionaires who want to live forever. Alas, I brought more than suspect supplements home with me—I’ve been out of action with a virus for the last few days.
I can’t really blame my fellow conference attendees for my illness, which doesn’t seem to be covid (a rapid antigen test was negative). I took a total of 13 trains to make it there and back, and heard more than a few coughs on the journey. And when I dropped my daughter off at nursery on Monday, I was told that every staff member was sick. For those of us in the Northern Hemisphere, it’s just that time of year.
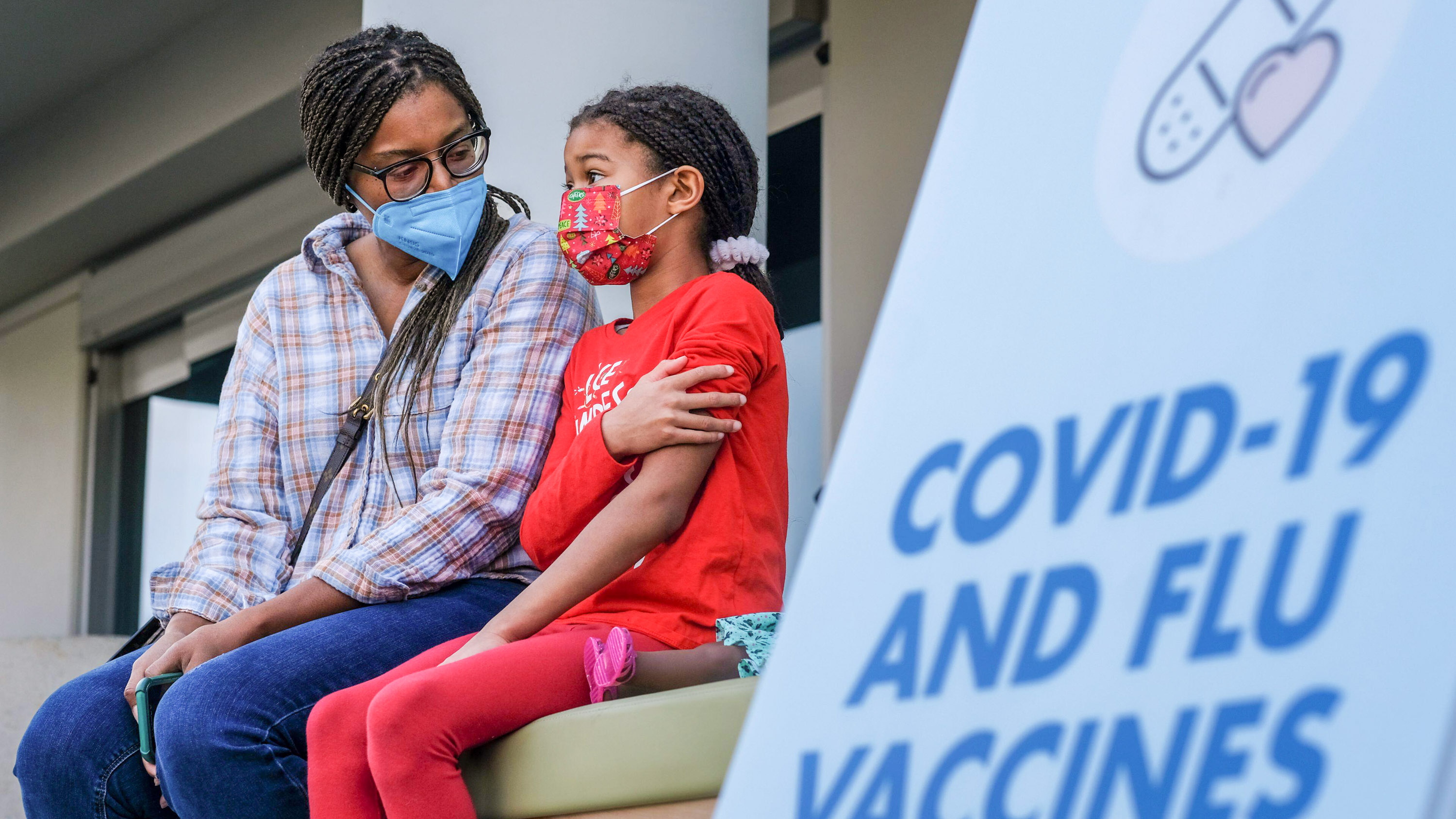
That’s partly why health authorities on both sides of the Atlantic are urging people to get vaccinated—against both the flu and covid-19. In recent months, we’ve heard warnings of a flu and covid “twindemic” on the horizon. Should we be worried?
A little bit. For a few reasons. First, people in the Northern Hemisphere are likely to be especially vulnerable to the flu virus this year because rates have been exceptionally low over the past two years.
The US typically sees tens of millions of flu cases every year, as estimated by the US Centers for Disease Control and Prevention. This estimate is drawn from the number of people hospitalized with the virus. In the 2018-2019 flu season, there were an estimated 29 million symptomatic cases, followed by 36 million the following year.
But in the flu season of 2020-2021, US hospitalizations were so low that the CDC wasn’t able to estimate the total number of cases at all. Flu activity was described by the organization as being “the lowest it has been since current reporting began in 1997.” Some epidemiologists worry that because we haven’t been exposed to the virus as much, we may have lost some immunity against it.
The downturn in cases had a lot to do with the covid-19 pandemic. All the measures that were put in place to stop the spread of the SARS-CoV-2 virus had the knock-on effect of minimizing the spread of other respiratory viruses, including those that cause flu.
The problem is that we’ve now dropped a lot of those measures. Most of us are now happily mixing in offices, transport hubs, pubs, and all the other places where infections can readily spread. Countries have reopened borders to international travelers—and while some require proof of covid vaccination, many don’t. No one checked my covid vaccination certificate as I traveled through England, France, and Switzerland.
Another notable feature of my journey was the distinct lack of face masks. While many epidemiologists still recommend wearing masks, especially in unventilated or busy indoor spaces, many countries have dropped official guidance on masking. In the 13 trains I took, I saw only around 10 people wearing a face covering.
Covid-19 outbreaks haven’t followed the same seasonal patterns as flu. But as we’ve seen multiple times over the past couple of years, the disease can mount a comeback when our defenses are low. We might be seeing the beginnings of a new wave here in the UK—the number of people testing positive for covid-19 increased by a staggering 42% in the last seven days, according to government figures. And if recent experiences are anything to go by, any surge in the UK could be followed a month or so later by a similar surge in the US.
The experiences of countries in the Southern Hemisphere provide another cause for concern. Flu season in Australia usually begins around May and peaks in October. This year, flu hit early and hard—peaking high in early June, according to the Australian government’s disease surveillance system. The outbreak hit after two years of exceptionally low flu activity, which is thought to have lowered immunity in the population. Most children under the age of two might never have experienced the flu before this year.
A drop in flu vaccination rates was also blamed for this year’s surge in cases in Australia. Here, the UK may be better placed to face the upcoming flu season—the proportion of eligible people over 65 receiving vaccines increased from 80.9% in the 2020-2021 flu season to 82.3% last season, safely above the WHO’s goal of 75% vaccination uptake.
But rates are much lower in the US, where only 66% of adults aged 65 or older received a vaccine during the last flu season. And the figure seems to have been in decline over the last few years.
That’s why the CDC, the WHO, and other health authorities are urging people to get vaccinated. It’s a familiar story, of course. But the fact is that people are still dying from both diseases—and those who are unvaccinated are at greatest risk.
As the weather cools in the Northern Hemisphere, and people increasingly mix indoors, we can expect cases to rise, Tedros Adhanom Ghebreyesus, director general of the WHO, told journalists at a press briefing on Wednesday. It’s not just the UK—several countries in Europe are already seeing increases in covid-19 cases, hospitalizations, and deaths.
Another cause for concern stems from the virus’s ability to evolve. The omicron variant is still responsible for the vast majority of cases globally. But the WHO is monitoring more than 300 omicron subvariants, all of which are considered to be “of concern.” As Maria Van Kerkhove, the WHO’s covid-19 technical lead, said at the same briefing: “We will continue to see waves of infection … because we will be living with this virus.”
Tech Review has been covering covid-19 since the pandemic began. Here are a few recent pieces from the archive:
- Covid-19 hit some much harder than others. We’ve only just begun to examine the racial disparities of long covid, as Elaine Shelly reports in this piece.
- And there’s still a big debate over long covid in children—with groups at loggerheads on the impact, and even the definition, of the illness, as I reported earlier this year.
- In China, a covid pop-up on your phone that requires you to get a PCR test could leave you quarantining for days for no apparent reason, my colleague Zeyi Yang reports.
- Two inhaled covid vaccines were recently approved for covid-19 in India and China, as I covered last month …
- … But the hunt is on for a universal covid vaccine based on nanoparticles, reports Adam Piore.
From around the web
Ever had your mind go blank? Brain scans show our brains can enter a neural state that makes it impossible to tap into our thoughts. (PNAS)
Doctors are discovering new, ultra-rare blood group systems—and have just described a 44th. (Wired)
Rapid antigen tests for covid-19 have paved the way for other home test kits—covering everything from flu to kidney disease. (Neo.Life)
The US shortage of Adderall—prescribed for attention deficit hyperactivity disorder (ADHD) and narcolepsy—is biting, with affected people saying their lives have been “turned upside down.” (Vice)
We’re becoming increasingly nearsighted. Myopia will affect half of the world’s population by 2050, partly because we’re spending more time reading indoors. (BBC Future)
Deep Dive
Biotechnology and health
How scientists traced a mysterious covid case back to six toilets
When wastewater surveillance turns into a hunt for a single infected individual, the ethics get tricky.
An AI-driven “factory of drugs” claims to have hit a big milestone
Insilico is part of a wave of companies betting on AI as the "next amazing revolution" in biology
The quest to legitimize longevity medicine
Longevity clinics offer a mix of services that largely cater to the wealthy. Now there’s a push to establish their work as a credible medical field.
There is a new most expensive drug in the world. Price tag: $4.25 million
But will the latest gene therapy suffer the curse of the costliest drug?
Stay connected
Get the latest updates from
MIT Technology Review
Discover special offers, top stories, upcoming events, and more.