A drug that cools the body’s reaction to Covid-19 appears to save lives
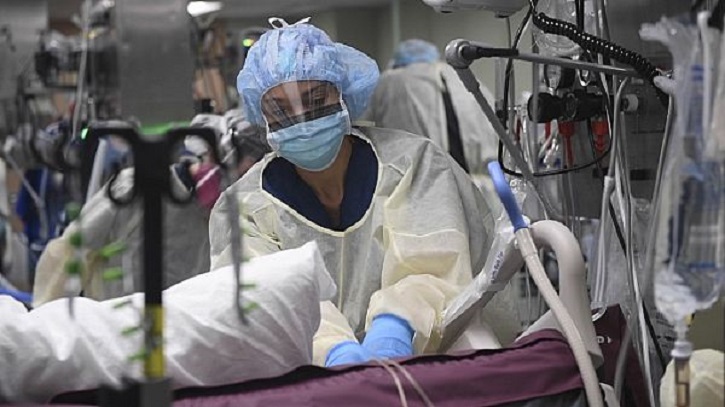
In an advance toward conquering covid-19, doctors in Michigan say an antibody drug may sharply cut the chance patients on a ventilator will die.
The problem: The pandemic viral disease is infecting millions, and for those who end up on a ventilator in an ICU, the odds are grim. More than half are dying.
The drug: Doctors at the University of Michigan set out to control the haywire immune reaction that pushes some covid-19 patients into a death spiral. To do it, they gave 78 patients on ventilators the drug tocilizumab, which blocks IL-6, a molecule in the body that sets off a reaction to an infection. (The drug is sold by Roche under the trade name Actemra.)
The result: The doctors say in a preprint that patients who got the drug were 45% less likely to die than those who didn’t. But there’s a big caveat, which is that the doctors knew which patients got the drug and which didn’t. Their picks for the drug-taking group could have been biased— people more likely to improve anyway, for example—so further studies are needed.
Emerging cocktail: In late May, Roche said it would start a trial to combine its IL-6 blocker with remdesivir, an antiviral drug with modest benefits that got emergency approval in the US for treating covid-19. That drug is meant to block the virus from replicating.
By combining the two drugs, doctors may be closing in on a cocktail able to cut the death rate from the virus, a step that would help society return to normal.
Deep Dive
Biotechnology and health
How scientists traced a mysterious covid case back to six toilets
When wastewater surveillance turns into a hunt for a single infected individual, the ethics get tricky.
An AI-driven “factory of drugs” claims to have hit a big milestone
Insilico is part of a wave of companies betting on AI as the "next amazing revolution" in biology
The quest to legitimize longevity medicine
Longevity clinics offer a mix of services that largely cater to the wealthy. Now there’s a push to establish their work as a credible medical field.
There is a new most expensive drug in the world. Price tag: $4.25 million
But will the latest gene therapy suffer the curse of the costliest drug?
Stay connected
Get the latest updates from
MIT Technology Review
Discover special offers, top stories, upcoming events, and more.