The high-tech medicine of the future may be biased in favor of well-off white men
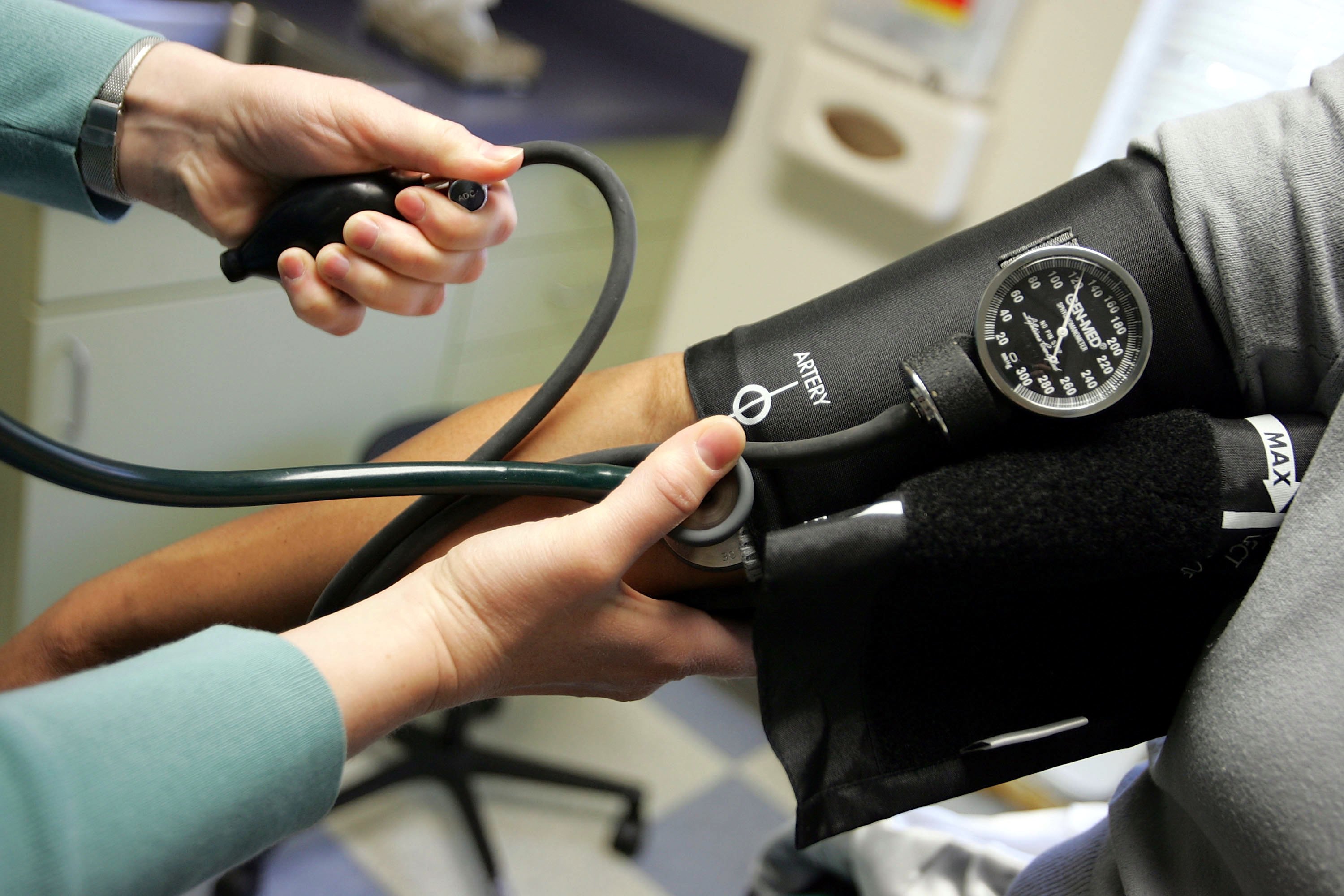
The promise of precision medicine is that all sorts of information about you—your genetics, ethnicity, diet, even neighborhood—could be used to create highly personalized treatments for whatever ails you, replacing the one-size-fits-all medicine of the past.
Doctors hope this will make everyone healthier. But a new report by the Data & Society Research Institute in New York says certain groups in the US are in jeopardy of being worse off when medicine is tailor-made. The one group notably not at risk: white men who can afford health insurance and a decent lifestyle.
So who stands to lose?
The uninsured. Precision medicine relies on researchers’ having lots of data. In the US, that data comes from electronic health records that doctors update when they see patients. Relatively little information gets collected about the uninsured and people who don’t see a doctor regularly. Those folks are most likely to be young adults and the poor.
The health-illiterate. A handful of big, ongoing precision-medicine studies are looking at people who wear electronic trackers to monitor their vital signs. Those people tend to be early adopters of technology. They’re likely to be physically active, interested in improving their health, well educated, and living near major cities. Researchers will need to find ways to get people who are less “health literate” to join such studies; otherwise precision medicine may end up mostly benefiting urban elites.
Women and minorities. These groups of people have often been excluded from medical research, so precision medicine that relies on historical data could be inherently biased. For example, guidelines for lung cancer screening in the US are based on a study of 53,000 people, only 4 percent of whom were African-American, according to Karriem Watson, a University of Chicago researcher quoted in the report. Similarly, what doctors know about cardiovascular disease comes mainly from research on men.
Immigrants. Some worry that the findings of precision-medicine research could be used to further discriminate against people who are already marginalized. Suppose, for instance, that researchers uncover a new health risk in a certain racial or ethnic group. Bioethicist Lisa Parker says we would then “have a health-related reason to limit those immigrants coming to this country and presenting a health burden for our health-care system.”
People in poor health. Because precision medicine would produce personalized health recommendations, it would be likely to put more responsibility on individuals to take charge of their own health. Those who do it best would be the “uncommonly tech savvy, highly health literate, self-directed, information seeking, English fluent, health focused, and well insured,” according to bioethicist Mark Rothstein, quoted in the report. Meanwhile, for people without resources and those already in poor health, the recommendations could feel confusing, overwhelming, and even intrusive, causing them to distrust the information they’re getting.
Deep Dive
Policy
A brief, weird history of brainwashing
L. Ron Hubbard, Operation Midnight Climax, and stochastic terrorism—the race for mind control changed America forever.
Africa’s push to regulate AI starts now
AI is expanding across the continent and new policies are taking shape. But poor digital infrastructure and regulatory bottlenecks could slow adoption.
Why the Chinese government is sparing AI from harsh regulations—for now
The Chinese government may have been tough on consumer tech platforms, but its AI regulations are intentionally lax to keep the domestic industry growing.
AI was supposed to make police bodycams better. What happened?
New AI programs that analyze bodycam recordings promise more transparency but are doing little to change culture.
Stay connected
Get the latest updates from
MIT Technology Review
Discover special offers, top stories, upcoming events, and more.