Unraveling the Mysterious Function of the Microbiome
What function does your microbiome play in your health? The answer is still a mystery, but emerging scientific evidence suggests it could have implications for treating many chronic diseases. A new class of microbiome drugs in development could eventually be effective against a range of hard-to-treat disorders, including gastrointestinal, metabolic, immunologic, and even neurologic problems.
The microbiome is a complex ecosystem of microbes that live in and among your body’s cells. It consists of distinct communities depending on where they live in the body. The microbe community in your mouth, for example, is different in composition from the one in your gut. Changes in the composition of the microbiome—for example, when pathogenic strains invade and push out “good” ones—have been correlated with with many diseases.
Most of the initial drugs in development are aimed at the gut microbiome, which is due to “some combination of its importance to key diseases and sampling ease,” says Peter DiLaura, CEO of San Francisco-based Second Genome. Tissue biopsies taken during colonoscopies and fecal samples are rich sources of information about the differences between the microbiomes of healthy and sick people.
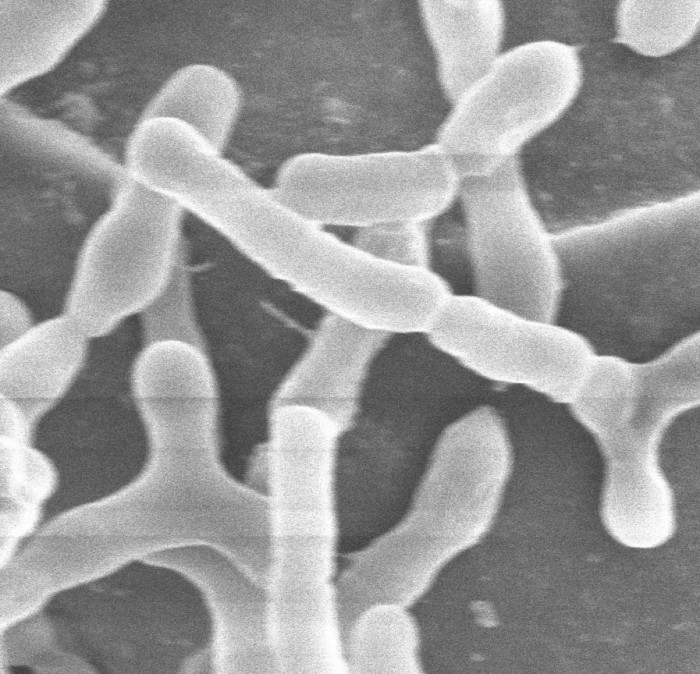
Some companies, led by Seres Therapeutics, are developing and testing drugs made of microbes. The idea is that adding carefully chosen species and strains of microbes can restore the gut microbiome’s healthy ecology, similar to the way fecal transplants are believed to work.
But DiLaura says it’s not clear yet whether the changes in the microbiome composition that are correlated with disease are driving that disease or are the effect of it. That’s why Second Genome is focused not only on the composition of the microbiome in healthy and sick people, but also its function, he says. Its first drug, which is in phase I clinical trials in the U.S., is for inflammatory bowel disease, a sometimes life-threatening condition characterized by inflammation of the intestinal lining or other parts of the gastrointestinal tract.
To better understand the microbiome’s function, the company’s scientists are studying the “dialogue” between the microbes and their human host. In some chronic conditions like inflammatory bowel disease, “there is some sort of cross talk between the microbiome and host that has persisted,” says DiLaura. Second Genome is aiming to “untangle” that cross talk.
In particular, “we’re looking at the things the bacteria are secreting”—the proteins, peptides, and metabolites the bacteria produce, says DiLaura. By sequencing the genomic information from the community of bacteria in tissue biopsies from both sick and healthy people, the company’s scientists can determine the “component pieces” of the dialogue between microbiome and host, helping them hypothesize about what is happening in disease, he says. They use techniques like machine learning to analyze terabytes of sequencing data and identify molecules that could be therapeutic, and then evaluate those candidate molecules in the lab.
Second Genome’s first drug prevents a specific molecule from binding to a receptor on the surface of cells lining the gut. The hypothesis is that it will block the inflammation that leads to inflammatory bowel disease.
A key challenge of grasping the functional differences between the microbiomes of inflamed and healthy tissue is deciphering the “interplay” between the relevant bacteria, says Marcus Claesson, a microbiologist at the APC Microbiome Institute in Ireland. How do the different strains interact, and how is that different in healthy people versus those with inflammatory bowel disease? It’s much easier to use genomic sequencing to elucidate which strains are present in the community than it is to investigate the collective function of the community, says Claesson, who is in the midst of an ongoing research collaboration with Second Genome.
Second Genome is also pursuing microbiome-based therapies for diabetes, which requires a discovery process that’s similar to the one for inflammatory bowel disease, says DiLaura. How is the composition and function of the microbiome different in people with diabetes? DiLaura says future microbiome medicines could be used against airway disorders and even diseases of the central nervous system.
Many factors go into these disorders. But the microbiome “is clearly playing some role, and we need to get to a better mechanistic understanding about how the microbiome and host are working together,” says DiLaura.
Keep Reading
Most Popular
Large language models can do jaw-dropping things. But nobody knows exactly why.
And that's a problem. Figuring it out is one of the biggest scientific puzzles of our time and a crucial step towards controlling more powerful future models.
How scientists traced a mysterious covid case back to six toilets
When wastewater surveillance turns into a hunt for a single infected individual, the ethics get tricky.
The problem with plug-in hybrids? Their drivers.
Plug-in hybrids are often sold as a transition to EVs, but new data from Europe shows we’re still underestimating the emissions they produce.
Stay connected
Get the latest updates from
MIT Technology Review
Discover special offers, top stories, upcoming events, and more.