The Science Surrounding Cryonics
Last month, the New York Times published a front-page article about Kim Suozzi and her decision, at the age of 23, to have her brain cryopreserved after learning she had terminal cancer. Her hope was to be able to preserve biological information that could someday be used to restore her mind, a practice known as cryonics. Michael Hendricks subsequently published a critique of this concept in MIT Technology Review (see “The False Science of Cryonics”). While his article focuses primarily on hypothetical brain “uploading” to computers, he and others have raised an intriguing question: can any technology, even in principle, preserve the unique features of an individual’s mind?
We agree there is more to the mind than the synaptic connections between neurons. The exact molecular and electrochemical features of the brain that underlie the conscious mind remain far from completely explored. However, available evidence lends support to the possibility that brain features that encode memories and determine behavior can be preserved during and after cryopreservation.
Cryopreservation is already used in laboratories all over the world to maintain animal cells, human embryos, and some organized tissues for periods as long as three decades. When a biological sample is cryopreserved, cryoprotective chemicals such as DMSO or propylene glycol are added and the temperature of the tissue is lowered to below the glass transition temperature (typically about -120 oC). At these temperatures, molecular activities are slowed by more than 13 orders of magnitude, effectively stopping biological time.
Although no one understands every detail of the physiology of any cell, cells of virtually every conceivable kind are successfully cryopreserved. Similarly, while the neurological basis for memory, behavior, and other features of a person’s identity may be staggeringly complex, understanding this complexity is a problem largely independent of being able to preserve it.
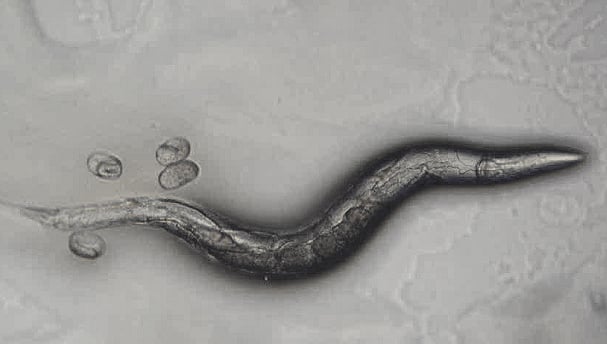
Direct evidence that memories can survive cryopreservation comes from the roundworm Caenorhabditis elegans, the very animal model discussed in Hendricks’s response. For decades C. elegans have commonly been cryopreserved at liquid nitrogen temperatures and later revived. This year, using an assay for memories of long-term odorant imprinting associations, one of us published findings that C. elegans retain learned behaviors acquired before cryopreservation. Similarly, it has been shown that long-term potentiation of neurons, a mechanism of memory, remains intact in rabbit brain tissue following cryopreservation.
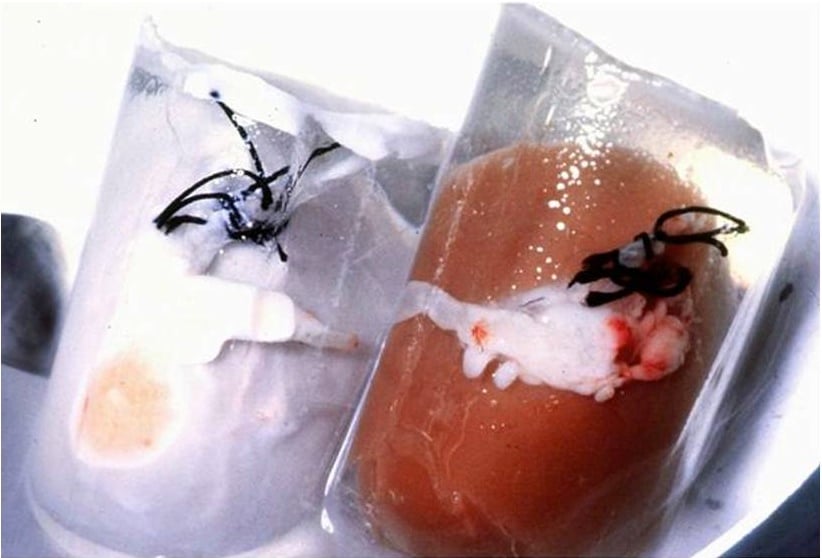
Reversibly cryopreserving large human organs, such as hearts or kidneys, is more difficult than preserving cells but is an active area of research with important public health benefits, since it would greatly increase the supply of organs for transplant. Researchers have made progress in this area, successfully cryopreserving and later transplanting sheep ovaries and rat limbs, and routinely recovering rabbit kidneys after cooling to -45 °C. Efforts to improve these technologies provide indirect support for the idea that the brain, like any other organ, may be adequately cryopreserved by current methods or methods under development.
For those who hope to preserve and restore the unique information-encoding features of the mind, a key question is when this information is actually lost following cardiac arrest. It is clear from examples of emergency resuscitation that information loss occurs not at the moment heart or brain activity stops, but when the chemistry or structure of life becomes irreversibly damaged—often significantly after clinical death has been established. For instance, although brain activity is suspended at temperatures below 18 °C, the medical literature contains many cases of people who have survived profound hypothermia without permanent brain damage. In one famous example, Swedish radiologist Anna Bågenholm was trapped under ice during a skiing accident and then resuscitated after being considered clinically dead for more than two hours.
Some surgical procedures also rely on intentionally arresting brain activity with the help of hypothermia. One of the authors’ institutions is carrying out a Defense Department-funded clinical trial to induce profound hypothermia (body temperatures of less than 10 °C) in critically injured trauma victims, effectively shutting the brain down and restarting it later to buy time to save the patient’s life.
It is easy to dismiss controversial practices such as cryonics and gloss over the research surrounding them, but we should remember and even respect that prevailing views are often shown to be incorrect, and that what is impossible now may be possible in the future. For example, Ignaz Semmelweis, the father of germ theory, was widely ignored when he proposed in the 19th century that nurses and doctors should wash their hands before treating patients. Even today, physicians are frequently incorrect when predicting outcomes in end-of-life situations.
Cryonics deserves open-minded discussion, as do mainstream efforts to understand the nature of consciousness, preserve human tissue and organs for life-saving transplants, and rescue critically injured patients by understanding the boundaries between biological life and death.
David W. Crippen is a professor in the Departments of Critical Care Medicine and Neurological Surgery, University of Pittsburgh.
Robert J. Shmookler Reis is a professor in the Departments of Geriatrics, Biochemistry & Molecular Biology, and Pharmacology/ Toxicology at the University of Arkansas for Medical Sciences.
Ramon Risco is a professor of engineering and director of the CryoBioTech Cryobiology Laboratory, University of Seville, and senior physicist at the National Accelerator Centre, Spain.
Natasha Vita-More is a professor and chair of graduate studies at the University of Advancing Technology.
Keep Reading
Most Popular
Large language models can do jaw-dropping things. But nobody knows exactly why.
And that's a problem. Figuring it out is one of the biggest scientific puzzles of our time and a crucial step towards controlling more powerful future models.
How scientists traced a mysterious covid case back to six toilets
When wastewater surveillance turns into a hunt for a single infected individual, the ethics get tricky.
The problem with plug-in hybrids? Their drivers.
Plug-in hybrids are often sold as a transition to EVs, but new data from Europe shows we’re still underestimating the emissions they produce.
Stay connected
Get the latest updates from
MIT Technology Review
Discover special offers, top stories, upcoming events, and more.