A Turning Point
When Robert Desimone was 18, he spent a month at a state mental hospital. He was there not as a patient but as a college freshman, on January break from Macalester College, who had been given the opportunity to live alongside and observe patients with schizophrenia and bipolar disorder. During that month, he got to know a patient in her 30s who suffered from schizophrenia. A promising college student before her diagnosis, she had not responded to any of the treatments.

“What was so frustrating was that here was an intelligent person who I could have imagined as a fellow student in college, and yet here she was stuck in this mental hospital because she had these delusional ideas,” Desimone recalls. “That really opened my eyes to how terrible some of the serious mental illnesses were, and how frustrating it was for the physicians trying to treat them.”
That was 45 years ago. And yet many of those same frustrations persist—especially the lack of effective, targeted treatments. Researchers in the 1950s through the early 1970s had stumbled upon compounds that proved useful in treating symptoms such as delusions. But because we still know little about how the brain works, most of the drugs developed since then are merely derivatives of those early treatments and no more effective. Instead of addressing specific brain circuits thought to be involved in the illness, they bathe the entire brain in chemicals, producing side effects for many patients. And for some, they don’t work at all.
Desimone, now the director of MIT’s McGovern Institute for Brain Research and the Doris and Don Berkey Professor of Neuroscience, believes that new technology and novel approaches to studying the brain will change all this. Genomic sequencing, optogenetics, and tools for precisely editing genes have given neuroscientists many new ways to understand what goes wrong in people with brain disorders so they can begin to identify potential treatment targets.
“With the much better understanding that we have of neural circuits and how they’re involved in specific sorts of behaviors and emotions, that will give us some leads on how we can manipulate those circuits in a way that can have a therapeutic effect,” he says. “If you knew exactly where the circuit was that needed to be modified, you could go right after it and not give a drug that’s going to affect everything in the brain.”
A shift to neuroscience
Desimone grew up in the suburbs of Philadelphia, where his mother worked in a department store and his father sold used cars in his grandfather’s dealership. He became interested in mental health during high school, when he read Joanne Greenberg’s I Never Promised You a Rose Garden and some books by Freud. His month living at the mental hospital convinced him that he wanted to become a clinical psychologist: during his time at Macalester, he studied psychology and worked as a counselor in a halfway house for those with mental illnesses, where he witnessed the hardships that patients and their families endured. “But frankly, I wasn’t very good as a counselor,” he says. “I took the ups and downs of the patients too personally.”
Instead, Desimone turned to neuroscience. For his PhD, at Princeton, he recorded neurons’ electrical activity to help identify cells in the brain that respond selectively to faces. Next, at the National Institute of Mental Health, he did animal studies to map the functions and connections of the brain’s cortex, which controls complex activities such as thought, attention, and sensory processing.
In 1998, NIMH director Steven Hyman appointed Desimone scientific director for its intramural research program—the institute’s internal research operation, which included about 65 labs. Desimone gave the program what Hyman calls a much-needed overhaul, bringing in new scientists and shutting down about half the ongoing clinical studies because they were not scientifically rigorous enough. That process “put the intramural program on the strongest footing it had been on for many years,” says Hyman, now the director of the Stanley Center for Psychiatric Research at the Broad Institute of MIT and Harvard, where he again works closely with Desimone.
Most of NIMH’s intramural research was devoted to clinical studies of new treatments, but as Desimone learned more about the research programs, he realized that there just weren’t very many promising options. The problem was that researchers didn’t really understand what’s happening in the brains of those with mental illness. “There wasn’t much in the pipeline,” he says. “I felt that we really needed to go back to the lab and concentrate more on fundamental knowledge of brain mechanisms and genetics.”
The frustrating lack of progress in clinical research hit home for Desimone in 2000 when he learned that his 16-year-old son had bipolar disorder. It had taken two years to arrive at the diagnosis, and the stark reality was that the treatments available were essentially unchanged from those used in the psychiatric ward where Desimone had lived more than three decades earlier.
His son’s illness reinforced Desimone’s drive to pursue neuroscience that could lead to better treatments. An opportunity to help guide that search arose in 2004 when he was asked to direct the McGovern Institute, which had gotten off the ground in 2000 under the leadership of MIT Institute Professor Phillip Sharp, HM ’96. Sharp had recruited the core faculty members and prepared for the move into Building 46, which had just been built to house the new institute as well as MIT’s Department of Brain and Cognitive Sciences and the Picower Institute for Learning and Memory.
Established by Lore Harp McGovern and the late Patrick McGovern ’59, the institute has a broad mission: to understand how the brain works and discover new ways to prevent and treat brain disorders. “When I was considering coming here and getting advice from people, there were people who thought that the McGovern Institute should be focused on one specific problem,” Desimone recalls. “However, I really felt that modern neuroscience is going to depend on interactions across levels, going from genes to neurons to circuits to brain systems and behavior. There’s just no way we’re going to be able to solve all these important problems by narrowly focusing on one little spot.”
Much of the McGovern Institute’s research focuses on mental illness. In 2012, nearly 44 million Americans adults—more than 18 percent of the adult population—suffered from mental disorders, including 9.6 million who had serious illnesses such as depression, schizophrenia, and bipolar disorder. “There are just so many people affected,” Desimone says. “In fact, most of us here [at the McGovern Institute] have family members or friends who have been affected by brain disorders, so we’ve all experienced this personally as well.” But he is confident that the institute is poised to make meaningful progress.
Technology revolution
Desimone feels fortunate to have arrived at the McGovern Institute “at a time when the field was about to explode with all the new tools from genetics,” he says. “I feel like I’m in the perfect place. We’re at the epicenter of all that’s happening in the field right now.”
One of the most promising approaches involves the use of optogenetics, which Feng Zhang, an MIT assistant professor who came to the McGovern Institute in 2011 and has a joint appointment at the Broad Institute, helped develop as graduate student at Stanford University. Optogenetics allows researchers to control specific neurons in lab animals, including rodents and primates. Using genetic engineering, they introduce light-sensitive proteins into the neurons they want to manipulate; then they pulse them with laser light to provoke or shut down the electrical impulses the neurons use to communicate with each other.
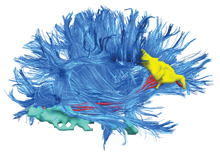
Zhang has used optogenetics to study brain cells involved in reward, a type of behavioral reinforcement often impaired in depression, while other neuroscientists at MIT have used it to decipher circuits associated with anxiety and compulsive behavior.
“Traditionally when we think about developing drugs to treat brain diseases, it’s all about this hypothesis that there’s some kind of chemical imbalance,” he says. “All the cells in the brain live in this milieu of chemicals, and if there’s an imbalance in the composition of the chemicals, then the brain has problems. But that’s a very gross and inaccurate way of thinking about how the brain functions. What optogenetics is starting to highlight is that abnormal signaling between different cells in specific neural circuits is probably underlying many of the neurological or psychiatric diseases that we know today.”
Zhang also happens to be a pioneer in the development of the genome-editing technology known as CRISPR, which is expected to play a huge part in deciphering the roles of different genes involved in mental illnesses. Genetic studies have revealed hundreds of variants linked with illnesses such as schizophrenia and autism. But figuring out the specific effects of particular variants has proved difficult.
Using CRISPR, researchers can systematically delete or add a specific genetic variant in lab animals to test its impact much more rapidly than previously possible. In a recent study, Zhang and Mriganka Sur, a professor at the Picower Institute, showed that they could use CRISPR in mice to study the functions of genes necessary for memory formation, as well as a gene associated with the developmental disorder Rett syndrome.
Most CRISPR research is being done in mice, but mouse models don’t always mirror what happens in a human brain. To more closely mimic mental disorders, McGovern researchers led by Desimone, Zhang, and Guoping Feng, a McGovern investigator and the Poitras Professor of Brain and Cognitive Sciences, have begun to use CRISPR to manipulate the genes of a new colony of marmoset monkeys housed at the facility. First they will try to breed monkeys with a condition similar to autism, and then they’ll move on to schizophrenia and other disorders. Once they have created these primate models, the researchers can begin the task of identifying treatment approaches. Desimone also hopes to get some pharmaceutical companies involved in this effort.
“A lot of the treatments that are tried out in mice seem very promising, and then they go into clinical trials and don’t go anywhere,” he says. “You hear the expression all the time that this is a great time to have Alzheimer’s disease if you’re a mouse. You could say the same thing about autism or any number of disorders. We’re hoping that the primate models will give us better testing and treatment platforms.”
Better diagnosis
In addition to developing better drugs, researchers hope to get better at identifying which patients are most likely to benefit from existing treatments. One way to do that is through brain imaging. John Gabrieli, a McGovern Institute member and professor of brain and cognitive sciences, uses two types of magnetic resonance imaging, functional MRI and structural MRI, to correlate brain differences with treatment responses.
In 2012, Gabrieli found that brain scans of patients with social anxiety disorder could predict whether they would benefit from cognitive behavioral therapy, a treatment that aims to change anxiety-producing thought patterns. Before treatment began, he scanned the patients’ brains with fMRI while they looked at images of angry or neutral faces. After 12 weeks, the patients who improved the most were those whose visual processing areas had shown a greater difference in activity when looking at the two types of faces.
Gabrieli is now working on using brain scans to distinguish between patients suffering from depression and bipolar disorder. “It takes an average of 10 years for bipolar patients to get the correct diagnosis, because their disorder can so easily resemble depression,” he says. “The treatments are so different that they are counterproductive if you give the wrong one to the wrong person.”
Other scanning techniques are helping McGovern researchers zero in on how the brain focuses. The institute’s Athinoula A. Martinos Imaging Center, which housed the first MRI scanner at MIT, became host in 2011 to one of the world’s few magnetoencephalography (MEG) scanners used for research. Whereas conventional MRI measures changes in blood flow, this type of scanner uses an array of hundreds of sensors encircling the head to measure magnetic fields produced by neural activity, revealing which parts of the brain are involved in a particular task. It can reveal the timing of neural activity down to the millisecond.
Desimone’s lab is using the MEG scanner to reveal how the brain shifts its attention from one type of object to another. In a study published in 2014, he found that when someone is looking at faces, the prefrontal cortex sends signals to a region that process faces; in someone looking at houses, it sends the signals to a brain area that interprets information about places.
“The work we do in my lab is really basic, but nearly every psychiatric disorder has an attentional component,” Desimone says. “For some disorders, even depression, one of the main complaints people have is they can’t focus. They just can’t get their minds focused on the task at hand, so they don’t get anything done.” He’s now using the MEG scanner to investigate the possibility of training people to control the brain interactions involved in focusing their attention.
Targeted treatments
All these new tools and approaches will help researchers launch a multipronged attack on mental illness, Desimone hopes.
“So far, almost all the treatments in psychiatry have been discovered serendipitously,” he says. “New genetic information has presented the neuroscience community with a huge challenge: to turn that genetic knowledge into treatments. Fortunately, neuroscientists now have a tremendous number of new tools for advancing that cause. If we had been handed this problem 10 or 15 years ago, we would have been in much poorer shape.”
A major step in that process will be developing animal models that accurately reflect human mental illness, as the McGovern researchers are trying to do with marmoset monkeys, Desimone says.
“Having just one of these genetic models look like it has a promising behavioral phenotype would be a huge milestone and show that this whole effort is moving in the right direction,” he says. If a potential drug treatment works in such animals, “that would really speed up moving it into human clinical trials,” he adds. “We’re keeping our fingers crossed.”
Keep Reading
Most Popular
Large language models can do jaw-dropping things. But nobody knows exactly why.
And that's a problem. Figuring it out is one of the biggest scientific puzzles of our time and a crucial step towards controlling more powerful future models.
How scientists traced a mysterious covid case back to six toilets
When wastewater surveillance turns into a hunt for a single infected individual, the ethics get tricky.
The problem with plug-in hybrids? Their drivers.
Plug-in hybrids are often sold as a transition to EVs, but new data from Europe shows we’re still underestimating the emissions they produce.
Stay connected
Get the latest updates from
MIT Technology Review
Discover special offers, top stories, upcoming events, and more.