Challenges Remain for Technologies to Fight Ebola
Technologies that might prevent the spread of Ebola beyond West Africa are under development, and work could accelerate if the outbreak continues to worsen. But even if a vaccine were available today, deploying it could prove surprisingly difficult.
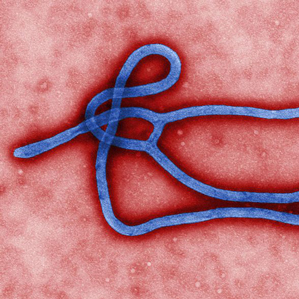
As of last week, the Ebola outbreak had claimed the lives of 88 percent of the more than 1,000 people who had contracted the virus. The virus causes fever, headache, sore throat, and other symptoms, followed by vomiting and diarrhea. It can lead to internal and external bleeding, and often death.
Ebola has affected relatively small populations in Africa since it was discovered in the 1970s. There has therefore been little incentive for companies to invest in developing treatments or vaccines, experts say. One treatment that has shown promise in animals but has not yet been tested in humans is called ZMapp—a combination of three monoclonal antibodies manufactured in tobacco plants by Mapp Biopharmaceuticals in San Diego. These antibodies are designed to mimic the antibodies the human body naturally produces as part of an immune response that’s typically disabled by the Ebola virus. The monoclonal antibodies attach to a part of the Ebola virus and trigger an immune response that neutralizes any virus particles floating around in the body to keep them from doing additional damage.
Samaritan’s Purse, the organization that employs one of the American Ebola patients, says that two American patients received this experimental serum while in Africa. MIT Technology Review was not able to reach Mapp Biopharmaceuticals or the Emory Hospital where the patient is being treated for comment. Several Ebola vaccine candidates are also in development, including one developed by the National Institute for Allergy and Infectious Diseases’ Vaccine Research Center that has shown promise in monkeys and has been fast-tracked for human testing this fall. The vaccine works by inserting two Ebola genes into a cell that helps to generate an immune response, allowing the body to recognize and fight the disease in the future.
Even if a vaccine is approved, however, one challenge would be figuring out who to vaccinate. “It’s not going to be all of Africa,” says Stephen Calderwood, chief of the Division of Infectious Disease at Massachusetts General Hospital. “It’s going to be in response to a specific outbreak and within a specific population that is at high risk, for example health-care workers.”
Furthermore, some reports say that there has been reluctance among patients in West Africa to accept care from Western doctors, stemming from a lack of trust in these health professionals.
Ebola is difficult to study because it occurs sporadically within small populations, compared to diseases like malaria or HIV. Animal models are used to help research the disease, and have offered clues as to why certain patients survive. For example, scientists have detected differences in the responses of monkeys that survive Ebola and those that die, such as the high prevalence of a subset of immune cells called neutrophils in the latter group, says John Connor, associate professor of microbiology at Boston University School of Medicine. “I’d say we’re in the middle of the story right now in understanding what the relevance of that is and why that’s the case,” he says.
Keep Reading
Most Popular
Large language models can do jaw-dropping things. But nobody knows exactly why.
And that's a problem. Figuring it out is one of the biggest scientific puzzles of our time and a crucial step towards controlling more powerful future models.
How scientists traced a mysterious covid case back to six toilets
When wastewater surveillance turns into a hunt for a single infected individual, the ethics get tricky.
The problem with plug-in hybrids? Their drivers.
Plug-in hybrids are often sold as a transition to EVs, but new data from Europe shows we’re still underestimating the emissions they produce.
Stay connected
Get the latest updates from
MIT Technology Review
Discover special offers, top stories, upcoming events, and more.