Mathematical Model Reveals Counterintuitive Way to Beat Multidrug Resistance
Stories of multidrug resistant tuberculosis, malaria, Streptococcus and such like fill our newspapers on an almost daily basis. There can hardly be a hospital in the Western world that isn’t affected by this problem.
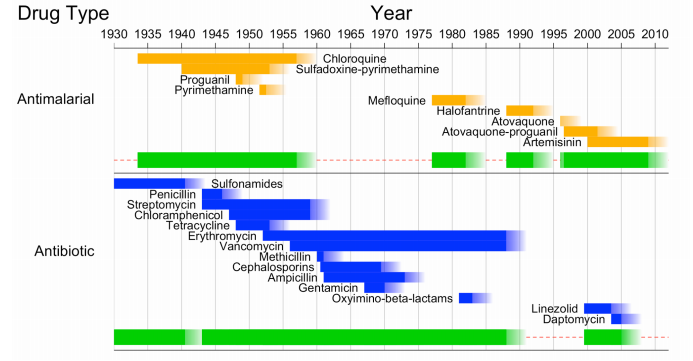
“Drug resistance is a serious public health problem that threatens to thwart our ability to treat many infectious diseases,” say Nathan McClure and Troy Day at Queen’s University in Canada.
So what to do. The current focus in the pharmaceutical world is to develop new drugs that take over when a pathogen has evolved resistance to the existing ones.
But there is another option. This is to reduce the rate at which pathogens evolve, which automatically increases the lifetimes of existing drugs.
The question is where to place the emphasis to ensure an adequate supply effective drugs for a given disease. Today, McClure and Day use a mathematical model to show that, all else being equal, the second of these approaches is always better. Their counterintuitive conclusion is this: “Slowing the evolution of drug resistance is more effective at ensuring an adequate supply of effective drugs than is enhancing the rate at which new drugs are developed”.
Here’s why. These guys first assume that a single drug is used to treat a disease until resistance evolves at which time a new drug is introduced, if one is available. So the total time over which the disease can be treated depends on two factors: the lifespan of each drug and the number of drugs used before resistance evolves.
McClure and Day study each of these factors separately. They show that reducing the rate of evolution has the same effect on the number of drugs used before resistance evolves as increasing the rate at which drugs are developed. In other words, both interventions are equally good in this respect.
However, increasing the rate of drug development has no effect on the lifespan of each drug. But reducing the rate of evolution obviously increases each drug’s lifespan. So in this respect, one intervention is dramatically better than the other.
That implies that slowing the evolution of resistance is inherently more effective than increasing the rate of drug development.
McClure and Day point out that if there is an upper limit to the number of drugs that can be developed for particular disease, then at some point drug development will always become effectively impossible.
What’s powerful about their new approach is that it applies even when there are no limits on drug development. “We show that even when there is no limit on the development of new drugs, slowing evolution is still inherently more effective,” they say.
That has profound implications for the way society appears to emphasise drug discovery over the management of evolution. “Although precise estimates are difficult to come by, it would appear that the research effort devoted to drug discovery currently far exceeds that devoted to resistance management,” they say.
But while it is straightforward to think of ways of increasing the rate at which new drugs are developed, by screening for new compounds for example, ways of slowing the evolution of resistance less well-known.
But they are still possible, say McClure and Day. They might include research into new strategies for reducing the inappropriate use of antimicrobials, determining when and where existing drugs should be used in combination versus as sequential monotherapies, as well as determining the optimal dose and timing of deployment for these existing drugs.
However, McClure and Day are careful to point out that the two different intervention strategies are not mutually exclusive—there is no reason to abandon one in favour of the other. Rather some optimal balance between them needs to be struck.
As things stand today, the balance is clearly not quite right. “A greater emphasis on evolution management might yield promising results for this pressing problem,” they conclude.
Ref: arxiv.org/abs/1304.7715: Slowing Evolution Is More Effective Than Enhancing Drug Development For Managing Resistance
Keep Reading
Most Popular
Large language models can do jaw-dropping things. But nobody knows exactly why.
And that's a problem. Figuring it out is one of the biggest scientific puzzles of our time and a crucial step towards controlling more powerful future models.
How scientists traced a mysterious covid case back to six toilets
When wastewater surveillance turns into a hunt for a single infected individual, the ethics get tricky.
The problem with plug-in hybrids? Their drivers.
Plug-in hybrids are often sold as a transition to EVs, but new data from Europe shows we’re still underestimating the emissions they produce.
Stay connected
Get the latest updates from
MIT Technology Review
Discover special offers, top stories, upcoming events, and more.