Predicting Cancer Drugs’ Impact
Devising the right chemotherapy regimen as soon as possible can spare cancer patients from painful side effects and increase their chances of survival. Two new imaging contrast agents could help by showing doctors whether a drug will reach the target tumor before it is administered.
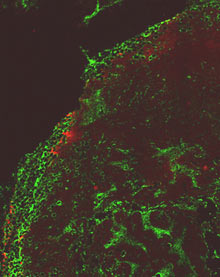
The first imaging agent can be used in combination with mammography to show doctors how well a commonly used breast-cancer drug will work, by quantifying the leakiness of a tumor’s blood supply. The imaging probe has been used to determine whether the drug will work in mice, and it’s on its way to clinical trials in humans.
Developed by Ravi Bellamkonda, a professor of bioengineering at Georgia Tech, and his colleagues, the imaging method is one of the first of its kind. The agent can be used to predict the effectiveness of a drug that has been one of nanomedicine’s early success stories. Marketed under the name doxil, it is a DNA-disrupting molecule encapsulated within a large lipid-and-polymer envelope. The envelope bulks up the drug to such a size that it cannot exit the blood stream and enter healthy organs, preventing side effects including liver and heart damage. But the drug can still get inside many tumors because their blood vessels are misshapen and leaky. The drug is currently used to treat several cancer types, including those of the breast and ovaries, but how well it works hinges on whether a tumor has enough leaky blood vessels to let it in.
“Though tumor sizes might be the same, the leakiness is all over the place,” says Bellamkonda. For a few years now, his lab has been using liposomes carrying iodine, which acts as a contrast agent, to image both tumor and healthy blood vessels. The liposomes are used with any imaging technique that relies on x-rays, including mammography and CT scans. Since the size and chemistry of the liposomes are similar to those of doxil and other lipid-enveloped drugs, Bellamkonda suspected that the imaging agents might interact with tumors in a similar way.
In a study published in this month’s issue of the journal Radiology, Bellamkonda’s research group describes using this contrast agent to quantify breast-cancer blood-vessel leakiness in mice. This, in turn, allowed the researchers to predict how successful doxil treatment would be. “We can predict if the drug will or won’t get there,” he says. Based on these predictions, the Georgia Tech researchers correctly predicted whether administering the drug would significantly shrink breast-cancer tumors in the mice.
It remains to be seen whether Bellamkonda’s imaging agent can help predict efficacy of other therapies, because many existing cancer drugs are smaller than the liposome particles. However, the bulky encapsulation used to make doxil is being developed for other cancer drugs.

“These probes might be useful for entire classes of drugs,” says Caius Radu, a professor of molecular and medical pharmacology at the University of California, Los Angeles, School of Medicine. Given the tremendous potential payoffs for patients, “there will be many [imaging agents] like this,” he predicts.
Radu’s own lab reported the success of a similar project this week, using a contrast agent visible on positron-emission tomography (PET) scans. The agent enters leukemia cells by the same mechanism as a drug used to treat the disease. Both the drug and the contrast agent enter tumors that express a particular protein, which normal cells do not produce. By tracking the imaging agent’s route through the body, the researchers can accurately predict whether the drug will extend the life span of mice with leukemia. His team describes these results in a paper published in the Proceedings of the National Academy of Sciences.
The chemistry of the two imaging agents is fundamentally different, but the philosophy behind them is the same. “We have to stop treating diseases and treat patients,” Radu says. Both groups hope that their imaging agents can help doctors pick the right therapy immediately, sparing patients from grueling drugs and the need to wait six months or so for conventional imaging results to show whether their tumor has shrunk.
Tailoring therapy is important, says Daniel Kopans, a professor of radiology at Harvard Medical School. However, he cautions, “don’t forget: this is in mice. Certainly many things that work in mice do not work in humans.”
Edward Graves, a professor of radiation oncology at Stanford Medical School, is also cautiously optimistic. The two new imaging agents are part of a growing number of probes that track cancer molecules inside the body. But most of these agents remain in preclinical or very early clinical tests. “No one knows how best to interpret this data in a clinical setting,” Graves says. “What implications do [these imaging signals] have for cancer progression and therapy?”
Bellamkonda says that a Houston-based startup called Marval Biosciences has agreed to license his group’s liposome-imaging technology. In 16 months’ time, the company plans to apply to the Food and Drug Administration for permission to test the imaging method in people. The University of California researchers hope to have enough data to move to human studies by the end of the year.
Keep Reading
Most Popular
Large language models can do jaw-dropping things. But nobody knows exactly why.
And that's a problem. Figuring it out is one of the biggest scientific puzzles of our time and a crucial step towards controlling more powerful future models.
How scientists traced a mysterious covid case back to six toilets
When wastewater surveillance turns into a hunt for a single infected individual, the ethics get tricky.
The problem with plug-in hybrids? Their drivers.
Plug-in hybrids are often sold as a transition to EVs, but new data from Europe shows we’re still underestimating the emissions they produce.
Stay connected
Get the latest updates from
MIT Technology Review
Discover special offers, top stories, upcoming events, and more.