A startup that marries AI with empathy is helping women conceive

When Shivani was nearing her 30th birthday, she realized she wanted to be a mom. She just wasn’t sure when. She didn’t yet have a long-term partner and was aware of her ticking biological clock. So she looked into freezing her eggs to increase her chances of having children later on in life. “No one has their eggs forever, unfortunately,” she says.
Shivani, who asked not to use her real name to avoid controversy in her Indian immigrant community, didn’t go through with it immediately—she felt the technology was too young and invasive. But around her 36th birthday, she felt she shouldn’t wait any longer. Having managed to save the $15,000 she estimated it would cost, she went and visited a clinic.
Before beginning the egg extraction process, a woman must first undergo an evaluation to determine her suitability for in vitro fertilization (IVF). Clinics often do this using a national registry of IVF outcomes to look up how many women within a patient’s age range successfully ended with a live birth. A fertility specialist then adjusts that percentage by factoring in the patient’s height and weight, as well as tests like ultrasounds and blood work.
Shivani began the process the same way: she reported her age, measured her body mass index, and took some tests. But when she returned to the clinic to discuss her prospects, her doctor began by handing her a multicolored report. It had been produced by feeding that information into a machine-learning algorithm and showed a personalized prediction for how her chances of having a baby would increase with each egg extraction cycle, up to three. It also showed her how she stacked up against other women who had been treated at the same clinic. “I already came in committed 100%, but the report put me at 120%,” she says. “It helped me solidify my decision.”
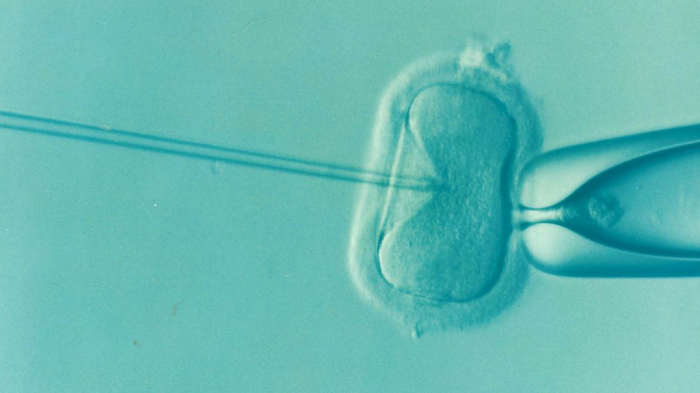
IVF can be a physically, emotionally, and financially taxing process that often requires multiple extraction cycles. More than 50% of those who start IVF drop out after the first failed cycle because of costs and uncertainty. Univfy, the company behind the software that produced Shivani’s report, believes machine learning can help people start and see the process through: by giving them more precise, personalized predictions of their possible outcomes. But that is only part of the solution. The other, equally important part: empathetic communication.
“For the vast majority of people in the United States, the biggest obstacle is that patients drop out before they get to the baby,” says Serena Chen, Shivani’s doctor, whose institution, the Institute for Reproductive Medicine and Science in New Jersey, uses Univfy’s software. “Patients need hope. Univfy is another tool where you can give them very solid, data-based information to say, ‘Keep going. You’re getting closer and closer to the baby.’”
Cofounded by two Stanford professors in 2009, Univfy spun out of a research project to use machine learning to produce more accurate IVF outcome predictions. Through several peer-reviewed studies, the researchers showed that even a basic machine-learning model could produce much more accurate IVF predictions than those made by clinics. This was because while clinics primarily rely on age-based aggregate statistics and a doctor’s intuition, the AI model could systematically factor in a patient’s relevant health data. The process was more rigorous and more personalized, and produced more refined predictions. Not only that, but age-based estimates often underestimated a given patient’s chances, giving her less confidence in her ability to proceed. “It’s not possible that two women would have the same probability of success just because they fall into the same age group,” says Mylene Yao, a cofounder and Univfy’s CEO.
Univfy works individually with each clinic that buys its service, training a relatively simple, bespoke machine-learning model using only the clinic’s local patient data. It allows the company to feed the algorithm whatever data the clinic has available—whether that means simple patient profiles with just their age, BMI, and health indicators or more complicated profiles with their clinical diagnoses, treatment procedures, and medical histories. Once a model is trained, a doctor can simply input a new patient’s test results and health indicators into Univfy’s software to produce an easy-to-read report.

When Chen first began using Univfy, she found that its predictions were often not far from her own, but that patients had a more positive experience when they received the report than when she tried to communicate similar information. “I think a huge part of it is the graphics and the fact that the patient gets to take this thing home with them and say, ‘This is my information,’” she says. “There’s a huge emotional component. Patients need certainty.”
Univfy now has partnerships with 20 clinics in the US and Canada across more than 50 locations. To date, Shivani is among 10,000 patients who have used its reports as part of their decision-making process; Yao says women who receive the report are on average twice as likely to proceed with treatment. Last year, the company raised $6 million to continue expanding their services. Yao is now working to better accommodate same-sex couples, who often seek more information about how a sperm donor or surrogate can affect their chances of success.
Chen describes Univfy as part of a new, welcome trend of health-tech startups that are helping empower patients with their own decision-making agency. The old-school medical model of a “man in a white coat” dictating what’s good for you is slowly going out the window. “I think Univfy has really improved outcomes and access to care,” she says, “because we are engaging the patient much more in the conversation and raising the bar for her understanding of her own situation.”
To have more stories like this delivered directly to your inbox, sign up for our Webby-nominated AI newsletter The Algorithm. It's free.
Deep Dive
Artificial intelligence
Large language models can do jaw-dropping things. But nobody knows exactly why.
And that's a problem. Figuring it out is one of the biggest scientific puzzles of our time and a crucial step towards controlling more powerful future models.
Google DeepMind’s new generative model makes Super Mario–like games from scratch
Genie learns how to control games by watching hours and hours of video. It could help train next-gen robots too.
What’s next for generative video
OpenAI's Sora has raised the bar for AI moviemaking. Here are four things to bear in mind as we wrap our heads around what's coming.
Stay connected
Get the latest updates from
MIT Technology Review
Discover special offers, top stories, upcoming events, and more.