A robotic catheter has autonomously wound its way inside a live, beating pig’s heart
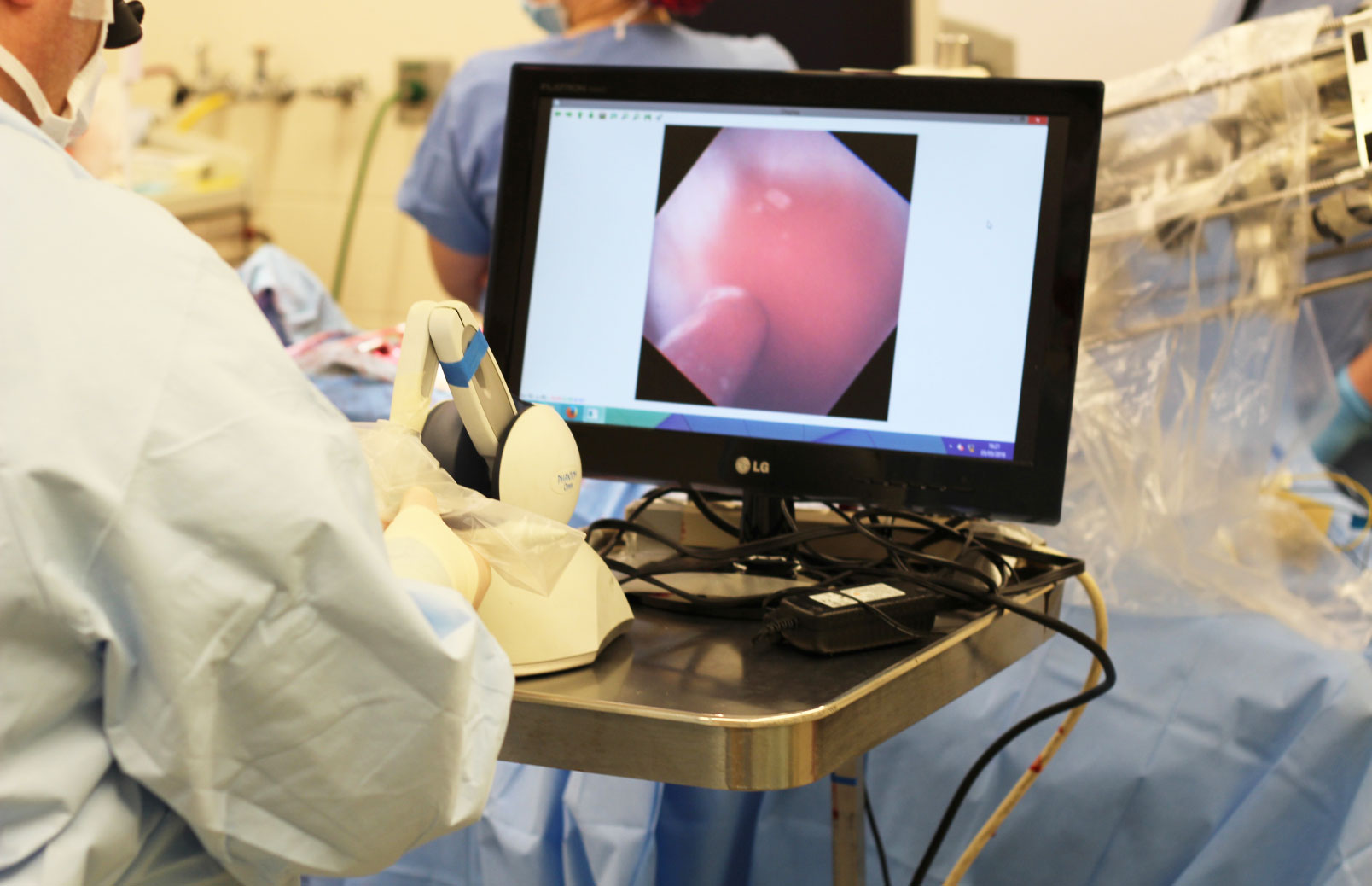
Operating inside a beating heart is a complex, delicate procedure that requires skilled surgeons. Medical personnel typically use joysticks and a combination of x-rays or ultrasound to carefully guide catheters through the body.
Now, for the first time, a robotic catheter has been able to autonomously navigate inside a heart to help carry out a particularly complex procedure. The device, which was inspired by the way certain animals learn about their surroundings, was used to help surgeons close leakages within the hearts of five live pigs.
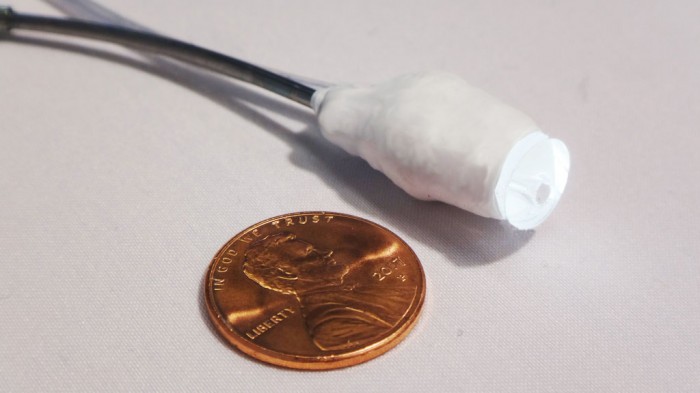
“Rats use whiskers to tap along the wall, humans feel their way, and cockroaches use their antennae,” says Harvard Medical School’s Pierre Dupont, who led the new study published in Science Robotics. “Similarly, this device uses touch sensors to work out where it is, and where to go next, based on a map of the heart.”
The device is 8 millimeters across, with a camera and an LED light on its tip that work as a combined optic and touch sensor. A machine-learning algorithm that was trained on approximately 2,000 heart-tissue images was used to guide it as it moved. The touch sensor periodically tapped against the heart’s tissue as the device wound its way through, helping it know where it was and making sure it wasn’t likely to damage the tissue.
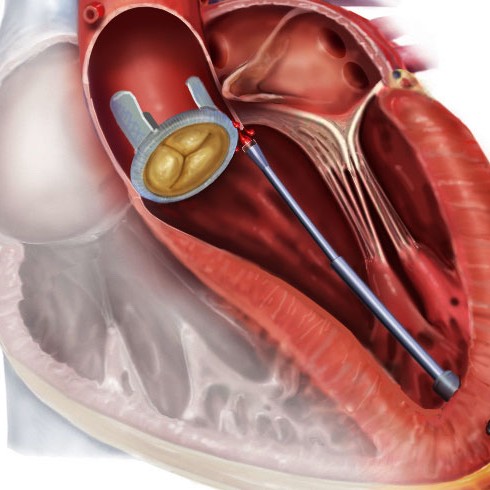
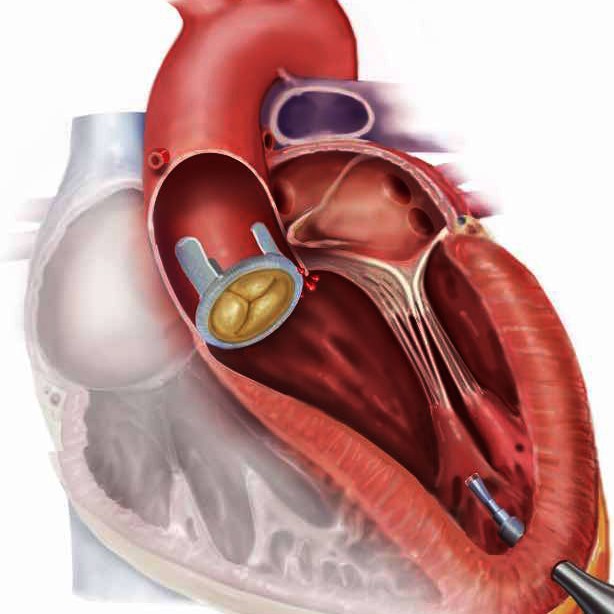
During the experiment, which involved 83 trials on five pigs, the catheter navigated to the correct location 95% of the time. That’s a similar success rate to what experienced clinicians achieve, and the procedure left no bruising or tissue damage, the research team said. Once the catheter was in position, the surgeons took control and carried out the procedure to fix the leak. Although robotic catheters have been available for some years, this is the first one that’s been able to find its way without human help.
The idea is that one day, such technology could free up surgeons to concentrate on other tasks or help less-experienced medical staff carry out more-complex procedures. The technology could be repurposed for use on humans within five years, says Dupont.
Deep Dive
Biotechnology and health
How scientists traced a mysterious covid case back to six toilets
When wastewater surveillance turns into a hunt for a single infected individual, the ethics get tricky.
An AI-driven “factory of drugs” claims to have hit a big milestone
Insilico is part of a wave of companies betting on AI as the "next amazing revolution" in biology
The quest to legitimize longevity medicine
Longevity clinics offer a mix of services that largely cater to the wealthy. Now there’s a push to establish their work as a credible medical field.
There is a new most expensive drug in the world. Price tag: $4.25 million
But will the latest gene therapy suffer the curse of the costliest drug?
Stay connected
Get the latest updates from
MIT Technology Review
Discover special offers, top stories, upcoming events, and more.