Gene therapy is saving children’s lives—but screening to discover who needs it is lagging behind
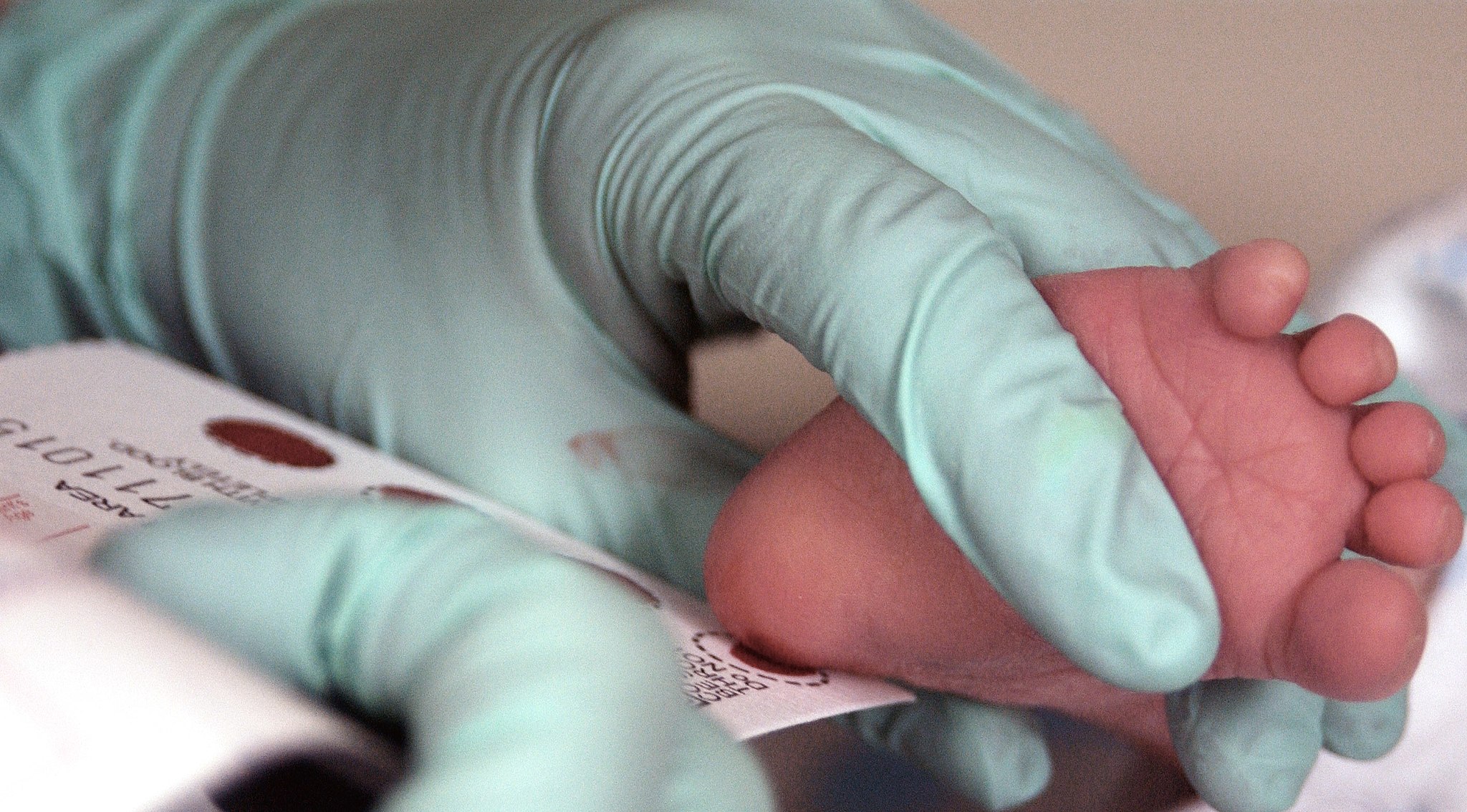
Fifteen children born with a rare muscle-wasting disease would probably not be alive today if not for an experimental treatment that tweaked their genes shortly after they were born.
The disease, called spinal muscular atrophy, would likely have killed most of them by age two. Amazingly, many of the children can now speak and sit on their own, and a few are even walking—milestones they never would have reached without the treatment. The company behind the drug, AveXis, is seeing the most dramatic results in children who are treated in the first month or two of life.
That means identifying patients as soon as possible—ideally at birth. Finding them early could mean the difference between life and death. But as AveXis and other biotech companies race to bring transformative gene therapies to market, states have been slow to adopt screening tests for genetic diseases that are, increasingly, treatable.
Newborn screening tests in the US cover a minimum of 34 disorders, and many states have opted to add more. Yet most don’t look for spinal muscular atrophy (commonly abbreviated as SMA), even though it’s the leading genetic cause of infant death. About 400 babies in the US are born with it every year. AveXis’s therapy is for the most common form, type 1.
For parents of children with SMA, like Khrystal Davis, newborn screening means giving those with the condition as close to a normal life as possible.
“These children shouldn’t have to live out life in a wheelchair when they could run, walk, and play,” says Davis, a founder of the Texas SMA Newborn Screening Coalition.
Time is of the essence in treating SMA type 1. A single mutation in the SMN1 gene causes swift and irreversible damage to a baby’s motor neurons, which are located in the brain stem and spinal cord. This damage leads to muscle weakness, and children eventually develop trouble swallowing and breathing.
Davis’s son, Hunter, who is now six years old, had already lost all movement at two weeks of age. Hunter is alive thanks to Spinraza, a breakthrough SMA drug approved in December 2016. Children who have received the drug have made remarkable recoveries. But it must be given through a spinal tap once every four months, for life. It costs a whopping $750,000 for the first year of treatment and $375,000 every year after that.
AveXis’s gene therapy is meant to be a one-time treatment, infused into a vein during a 60-minute procedure. It uses an engineered virus to deliver healthy copies of the SMN1 gene to cells throughout the body. Once there, the new gene starts making a protein that’s essential for the survival of motor neurons.
If you wait, however, “the children have limited motor neurons for the gene therapy to get into and work effectively,” says Sukumar Nagendran, AveXis’s chief medical officer.
On average, the 15 children in the AveXis trial received the gene therapy four months after birth. They all responded, but Nagendran says two children who got it within the first two months of life had the most dramatic improvement; they’re now able to walk independently.
In April, AveXis began a new study, this time treating babies immediately after birth. The results will be able to tell researchers just how much better patients fare when they get the drug as newborns.
Other gene therapies may also work better in children before a genetic defect has time to irreparably damage the body. For example, Bluebird Bio is developing one that halted a deadly brain disorder called cerebral adrenoleukodystrophy (ALD), also known as Lorenzo’s Oil disease, in 15 out of 17 children. In a statement provided to MIT Technology Review, the company said outcomes are better when patients are treated before symptoms appear.
State by state
On February 8, a national committee that oversees newborn testing voted to recommend that SMA be added to the recommended universal screening panel. The next step is for the secretary of the US Department of Health and Human Services, Alex Azar, to sign off.
Even then, rolling out SMA screening for every newborn isn’t a done deal. A recommendation put forth by the committee is just that—a recommendation. It’s only binding in two states, California and Florida. Other states may choose to adopt the proposal or not.
Adding new diseases to screening rosters inevitably means adding to the cost of tests for newborns, which run about $110 to $150, depending on the state. The tests are typically covered by insurers or Medicaid, but funding in some states comes from the health department’s budget. Adding SMA would cost anywhere between 10 cents and $1, according to a report issued by the US government in March.
ALD, meanwhile, was recommended for addition to the federal list of screenings by the HHS secretary in 2015, but states have been slow to adopt the change. Only a handful test for it today.
“It’s a nightmare,” says Maria Kefalas, a patient advocate and founder of the Calliope Joy Foundation, which raises money to help children with leukodystrophy. “Lobbying states one by one is ridiculous.” Her daughter was diagnosed at age two with a rare genetic brain disorder called metachromatic leukodystrophy. An experimental gene therapy available at a single site in Milan, Italy, has saved children with the otherwise terminal disease—but only if it’s given early enough. London-based Orchard Therapeutics is working on commercializing the therapy.
To know or not to know
Not everyone thinks screening newborns for more diseases is a good idea. The results could cause extra anxiety for parents, and there’s the possibility of false positives.
A pilot program in Massachusetts that’s testing newborns for SMA, for example, showed that a baby had the disease—but a few months later it turned out to be a false alarm.
“Can you imagine what that couple went through?” says Kathryn Swoboda, a pediatric neurologist at Massachusetts General Hospital, who is involved in the pilot program. “It’s really tough on families.”
Not all parents want to find out if their child will go on to develop a serious disease, especially if, as in some cases, its onset is years away. SMA is a prime example: there are five types, and while most cases appear within the first six to 18 months of life, one type doesn’t come on until adulthood. Similarly, onset for cerebral ALD, which the Bluebird therapy is designed to treat, can occur when a child is anywhere between two and 10 years old. Swoboda says knowing this could make it harder for parents to bond with a child.
Still, people like Kefalas think the benefits often outweigh the risks. “There are so many ramifications of having this information at birth,” she says, “but for some diseases it seems like a no-brainer.”
Deep Dive
Biotechnology and health
How scientists traced a mysterious covid case back to six toilets
When wastewater surveillance turns into a hunt for a single infected individual, the ethics get tricky.
An AI-driven “factory of drugs” claims to have hit a big milestone
Insilico is part of a wave of companies betting on AI as the "next amazing revolution" in biology
The quest to legitimize longevity medicine
Longevity clinics offer a mix of services that largely cater to the wealthy. Now there’s a push to establish their work as a credible medical field.
There is a new most expensive drug in the world. Price tag: $4.25 million
But will the latest gene therapy suffer the curse of the costliest drug?
Stay connected
Get the latest updates from
MIT Technology Review
Discover special offers, top stories, upcoming events, and more.