Why HPV Vaccination Rates Remain Low in Rural States
Mandi Price never thought she’d be diagnosed with cancer at age 24. She was a healthy college student finishing her senior year when, during a regular Pap smear, her gynecologist found abnormal cells in her cervix. It was stage II cervical cancer.
Even more devastating was the fact that her cancer was preventable. Doctors detected a strain of human papillomavirus, the most common sexually transmitted infection in the U.S., in Price’s cancer cells. That strain of HPV is targeted by a vaccine called Gardasil. But Price never got the vaccine. Her primary care doctor in Washington state didn’t recommend it when she was a teenager. Had she received it before becoming infected with HPV, she might not have gotten cancer.
Price dropped out of her classes to get treatment. She needed surgery to remove the tumor from her cervix, then underwent chemotherapy and radiation to kill any remaining cancerous tissue. At her one-year follow-up appointment, doctors found that the cancer had spread. She endured chemotherapy for another six months. Now, at 29, Price is in remission and is working in Los Angeles. “Most of my 20s comprised being in a hospital. It was isolating,” she says.
Merck’s Gardasil vaccine was considered a breakthrough when it was approved by the U.S. Food and Drug Administration in June 2006. It was the first vaccine to protect against several cancers. But more than a decade after the vaccine came out, vaccination rates in many places in the U.S., especially in the South, Midwest, and Appalachian states, still remain much lower than rates for other childhood vaccines—too low to stop transmission of the most dangerous HPV strains.
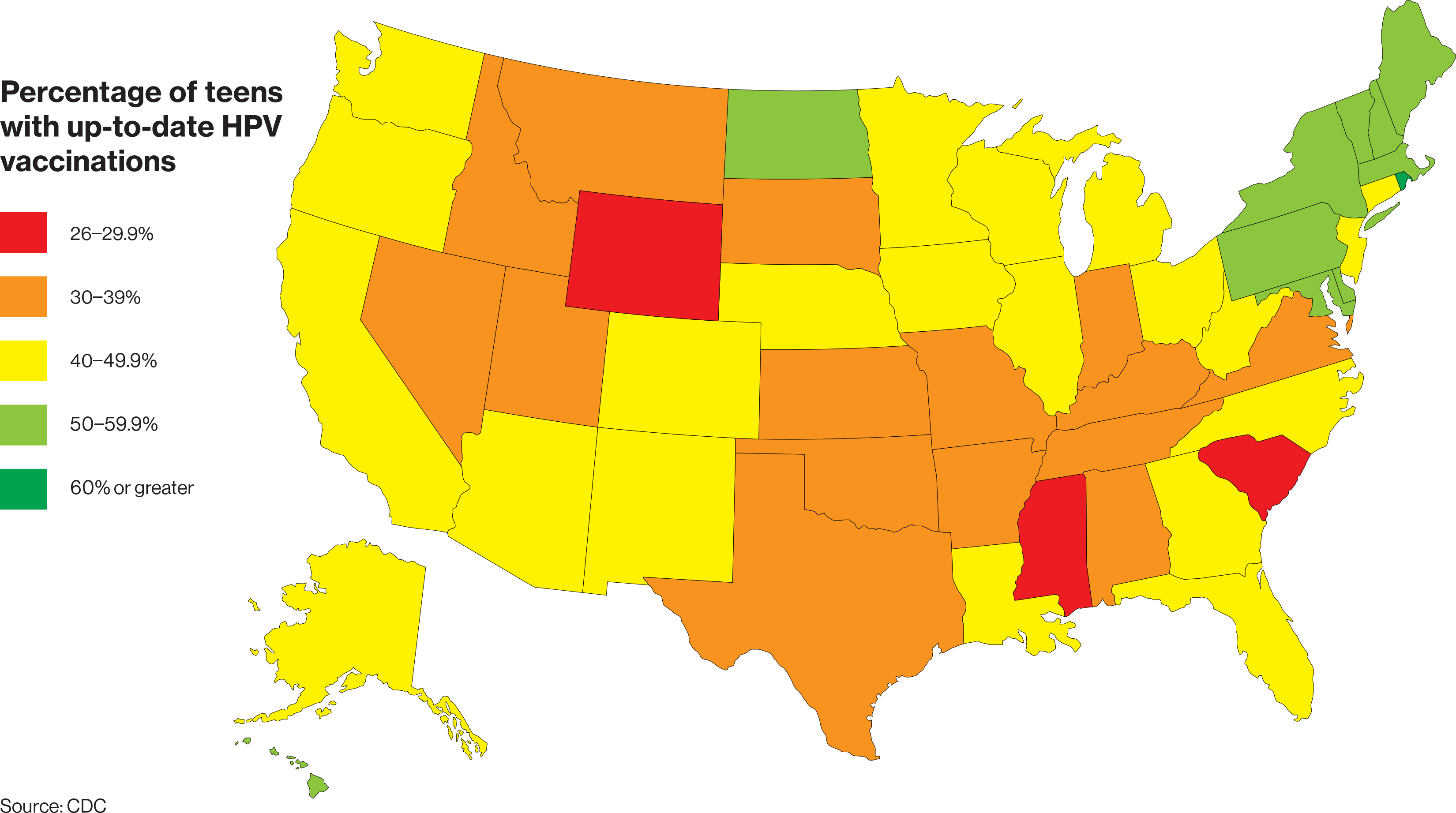
In 2016, only about 50 percent of girls and 38 percent of boys had all the required doses of the HPV vaccine needed to be fully protected, according to data released last week by the U.S. Centers for Disease Control and Prevention. Those figures are up slightly from last year, but still not close to the 80 percent that public health experts want to achieve.
Gardasil is approved to protect against cervical, vulvar, and vaginal cancers in girls and women ages 9 through 26, as well as anal cancer for the same age group in both girls and boys. Recently, the vaccine has also been shown to protect against oral cancers in men. HPV causes about 32,000 cancers every year, with cervical cancer the most common for women and oral cancers the most frequent in men.
Electra Paskett, a cancer epidemiologist at Ohio State University, says she is still surprised that the vaccine’s uptake has been so slow. “It’s crazy that there’s not a line around the corner. If we said we have a vaccine for breast cancer, we’d be vaccinating day and night,” she says.
The problem the vaccine has faced is its link to a taboo in American culture: sexual activity among teenagers. About one in four people in the U.S., including teens, are currently infected with HPV. Health-care providers are the biggest hurdle to getting more children vaccinated. Some primary care physicians, like in Price’s case, may not recommend it at all.
For Merck, the world’s largest vaccine maker, Gardasil has been a profit generator even though the company admits the uptake of the vaccine has been surprisingly slow. The company says it’s trying to increase rates by educating health-care providers.
William Schaffner, a professor of preventive medicine and infectious diseases at Vanderbilt University, remembers the initial excitement in the medical community when Gardasil first came out. “I thought the advent of our first explicitly anti-cancer vaccine, and the fact that it was so incredibly successful and safe, would be immediately embraced with pizzazz and rose petals,” he says.
Regional differences
State vaccination rates were as high as 73 percent among girls in Rhode Island and as low as 31 percent in South Carolina for all three doses in 2016. Among boys, Wyoming had the lowest rate, with only 20 percent getting the full round of shots.
Overall, teens living in major metropolitan areas were far more likely to get the vaccine than those living in rural areas, which may be more socially conservative and lack access to certain health-care services. In some of these places, average household incomes are lower than the national average, and parents might not be able to afford to take their pre-teens or teens to get the vaccine.
In some states with low vaccination rates, HPV-caused cancers are the among the highest. In Mississippi, for example, only about 34 percent of girls and 25 percent of boys get all required doses of the vaccine. The state also has one of the highest rates of HPV-related cervical cancer in the country. Wyoming tells a similar story, with high rates of HPV-associated cancers in both men and women.
Of course, those cancer rates can’t yet be tied to the states’ low vaccination rates. Gardasil was introduced just over a decade ago, and many of these cancer cases are in people who were too old to get the vaccine when it came out. But it means that these disparities could grow if more people there don’t get the vaccine.
HPV vaccination for boys is especially lagging in some areas. Paskett, who has studied cancer in Appalachia, say there’s a perception that HPV only causes cancers in women. “A lot of parents don’t know that boys should be vaccinated,” she says. Boys and men not only carry HPV but can get HPV-related cancers, like anal, penile, throat, and tongue cancers.
Price says shortly after her cancer diagnosis, she urged her parents to get her two younger brothers vaccinated.
Doctor hesitancy
A 2015 study found that a little over a quarter of the 776 pediatricians and family physicians surveyed do not strongly endorse the HPV vaccine. About one-third of the total doctors surveyed also said that having to talk about a sexually transmitted infection makes them uncomfortable.
Nneka Holder, associate professor of adolescent medicine at University of Mississippi Medical Center, says she is frustrated that so many doctors don’t recommend the HPV vaccine because they think it means they have to talk to parents about sex.
“We don’t usually explain to patients how they get hepatitis or meningitis,” she says. “So why should HPV be different?” Instead, she says health-care providers should focus on the cancer prevention aspect of the vaccine, rather than how HPV is spread.
Even health-care providers who do talk to parents about the vaccine aren’t always effective at getting their message across. A study from 2014 found that 47 percent of Minnesota health-care physicians and nurses that did ask parents about their concerns with the vaccine said they lacked time to probe the issue further, and 55 percent felt they couldn’t change parents’ minds.
Schaffner says doctors that are most successful with getting parents on board with the HPV vaccine are the ones who don’t call special attention to it. He says the best tactic is for physicians to sandwich in the HPV vaccine with other recommended vaccines—as in, “It’s time for your son to get the meningococcal, HPV, and Tdap vaccines.”
Parent concerns
Since the vaccine is just over 10 years old, it’s too early to know how many cases of cancer it has prevented so far. But clinical trials have showed that the vaccine provides nearly 100 percent protection against cervical infections caused by certain strains of HPV. These infections have fallen by 64 percent among teen girls in the U.S. since 2006, when the vaccine was introduced. Large clinical trials of the HPV vaccine have also shown it’s safe for both boys and girls.
These benefits have led Virginia, Rhode Island, and Washington, D.C., to adopt public school mandates for HPV vaccination. But some parents are still uncomfortable about the HPV vaccine’s association with sex and think their children don’t need it because they’re not sexually active. That has led parents to form groups in opposition to such mandates.
Aimee Gardiner, director of one such group called Rhode Island Against Mandated HPV Vaccine, says she doesn’t see HPV as the “epidemic” she thinks the CDC has made it out to be. “For me the risk of developing a cancer from any HPV is so insignificantly small that I do not feel like the vaccine is a necessity,” she says. Gardiner has two children, one of whom isn’t old enough to receive the vaccine and the other who hasn’t received it. She says she doesn’t plan to vaccinate them with Gardasil.
It’s true that for most people, the immune system clears the virus from their systems naturally. But for a small number of people, HPV persists and can turn cancerous. For those patients, like Price, cancer can be a major life ordeal, not to mention much more expensive than a vaccine that costs about $150 per dose.
Looking ahead
HPV vaccination rates continue to increase steadily, but the problems associated with its uptake could spell trouble for other vaccines in the future. For example, researchers for years have been working on a vaccine that would protect people from contracting HIV, the virus that causes AIDS. If a vaccine for HIV were ever to be successful, it could run into the same problems. HIV’s risk factors—unprotected sex and intravenous drug use—make it even more taboo.
Another worry is that rising anti-vaccine sentiments causing parents to opt out of vaccinating their children will hurt efforts to expand HPV vaccine coverage.
One factor that may increase vaccination rates is a new guideline from the CDC announced in October 2016. Children ages 11 to 14 now only need two doses of the HPV vaccine at least six months apart instead of three, which was previously recommended. Teens 15 and older still need to complete the three-dose series. This change may increase uptake of the vaccine, as vaccination rates drop off after each dose.
For Price and other cancer patients, the thought of not getting a vaccine that could prevent something so terrible is unimaginable. “I am a huge proponent of it,” she says. “If you had the chance to prevent cancer in your son or daughter, why wouldn’t you do that?”
Deep Dive
Biotechnology and health
How scientists traced a mysterious covid case back to six toilets
When wastewater surveillance turns into a hunt for a single infected individual, the ethics get tricky.
An AI-driven “factory of drugs” claims to have hit a big milestone
Insilico is part of a wave of companies betting on AI as the "next amazing revolution" in biology
The quest to legitimize longevity medicine
Longevity clinics offer a mix of services that largely cater to the wealthy. Now there’s a push to establish their work as a credible medical field.
There is a new most expensive drug in the world. Price tag: $4.25 million
But will the latest gene therapy suffer the curse of the costliest drug?
Stay connected
Get the latest updates from
MIT Technology Review
Discover special offers, top stories, upcoming events, and more.