U.S. Panel Endorses Designer Babies to Avoid Serious Disease
Since its invention four years ago, a powerful and precise technology for editing DNA called CRISPR has transformed science because of how it makes altering the genetic makeup of plants and animals easier than ever before.
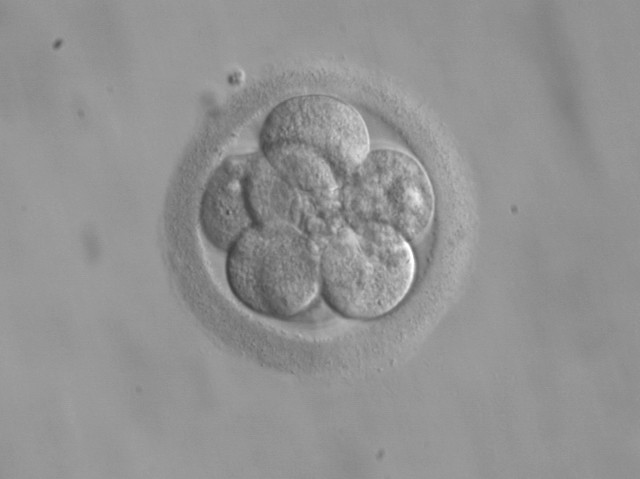
But no possibility opened by gene-editing technology has been so exciting, frightening, or as hotly contested as its capacity to allow humanity, for the first time, to control the genetic constitution of children by applying CRISPR to human embryos, sperm, or eggs—cells which together make up the “germ line.”
On Tuesday, in a striking acknowledgement that humanity is on the cusp of genetically modified children, a panel of the National Academy of Sciences, the nation’s source of blue-ribbon advice on science policy, recommended that germ-line modification of human beings be permitted in the future in certain narrow circumstances to prevent the birth of children with serious diseases.
"Heritable germline genome editing trials must be approached with caution, but caution does not mean that they must be prohibited," according to a 216-page report released today and which was researched and written over the course of a year by a 22-member panel of prominent scientists and experts.
The recommendations came freighted with moral and technical caveats, however. The panel believes it will be many years before germ-line engineering is safe enough to consider. The panel also said it should proceed only under “stringent oversight,” and drew a bright line between preventing disease and “enhancements” like attempting to alter genes to make people more intelligent, which it said should not be pursued “at this time.”
Despite the cautious language, the panel’s endorsement of GM humans could prove politically explosive, and puts the academy’s experts in conflict with existing legislation in Europe and the U.S. as well as with swaths of the public who oppose the idea of modifying the human genome from birth out of religious conviction or for other reasons.
Germ-line modification is already prohibited as a practical matter in the U.S. In 2015, pro-life legislators added a rider to the U.S. Department of Health and Human Services appropriations bill, which forbids the U.S. Food and Drug Administration from considering any proposal to create genetically modified offspring.
The legislation, which has to be renewed periodically, means that any proposal to modify an embryo and create a child would be ignored and could not legally proceed in the U.S.
In contrast, the academy panel argued that germ-line editing should be allowed in narrow cases where it is the only option for “preventing a serious disease or condition.” For instance, a couple who each suffers from beta thalassemia might only have healthy children free from the inherited blood disorder if they were able to produce embryos in which the genetic defect was corrected using gene editing. The report acknowledges that such circumstances might be exceedingly rare.
“They show a narrow but clear path to future clinical use,” says Tetsuya Ishii, a bioethicist at Hokkaido University in Japan who tracks global legislation on germ-line modification. He says the report also provides a justification for laboratory research already occurring in China, Sweden, and the U.K. in which gene-editing is being applied to human embryos to explore its potential. “They want to show that basic research toward severe disease prevention would be permissible,” he says.
The report’s authors struggled with how legitimate medical applications could be encouraged while still preventing “a slippery slope toward less compelling or even antisocial uses” like enhancement of height, looks, or intelligence. The report’s authors addressed that problem by arguing that no form of germ-line editing should be allowed if a country’s regulators can’t also guarantee the technology won’t be misused for “enhancement” of human beings.
“They have said there is one narrow corner, a tiny fraction of cases, where it might be the right thing to do,” says Eric Lander, head of the Broad Institute in Cambridge, Massachusetts, which has invested heavily in developing CRISPR technology. “What is fascinating is their argument that if we can’t control where it goes from there, we shouldn’t do it at all.”
It’s not clear how such a policy, which Lander calls “the ‘no slippery slopes’ recommendation,” would be implemented. Other technologies considered dangerous, like nuclear weapons, are monitored by a complex combination of technical bodies, international diplomacy, sanctions, and military threats.
Lander says the Broad Institute is “uneasy” with germ-line therapy. It controls more than a dozen patents on CRISPR, which it has licensed to biotech companies, but with a requirement they don’t use it for germ-line modification. “We didn’t want to be licensing technology for germ-line editing ahead of society reaching consensus and we are still very far from a consensus,” Lander says.
The report draws a sharp distinction between modifying embryos and modifying the DNA of adults and children. The latter process, known as gene therapy, is already a well-established part of medical research, does not raise the same ethical questions, and should proceed without new restrictions. Scientists are now racing to apply CRISPR as an even more effective way to perform gene therapy on adults, including to treat cancer and muscular dystrophy.
In the case of editing human embryos, the line between avoiding serious disease and enhancement may eventually prove to be a blurry one. In addition to preventing the transmission of known genetic diseases like beta thalassemia or cystic fibrosis, the report’s authors said their positive recommendation could also apply to genetic improvements that would act like a vaccine, making people less susceptible to HIV infection or cancer. For instance, people with a certain version of a gene called ApoE are much less likely to develop Alzheimer’s. The report’s authors said that swapping in a “protective” version of ApoE or another gene to an embryo might also be considered acceptable if it prevents disease.
“We do not view prevention as a form of enhancement,” says R. Alta Charo, a University of Wisconsin bioethicist who co-chaired the panel. “But whether it’s permissible is up to regulators.” She says the group intentionally did not list specific diseases or situations where germ-line modification should be used.
Controlling the technology could prove difficult. One worry is that doctors and scientists will go overseas to countries with permissive rules, or no rules, to attempt it. That is already occurring with a related technique known as mitochondrial transfer, which involves the transfer of DNA-bearing structures between eggs. Last year, a New York fertility doctor treated an American woman in Mexico using the procedure.
Most reports of the academy quickly end up on bookshelves and are of interest to only a few experts. But George Annas, a bioethicist at Boston University, says this one has the potential to be politically explosive because of how it presents the right of parents to use germ-line modification as a “procreative liberty” such as abortion.
“The scientists are saying this is all a question of risk benefit analysis, versus saying, 'No, it’s just wrong to do,'” says Annas. He thinks the committee “underestimates” public discomfort with the idea. “It’s like torture—some people think we should never do it, other people say, 'No, no, if it works, then it’s okay.' Designer babies is a lot like that.”
Charo says her panel did not consider the political ramifications of its findings. “We looked at these questions without considering what happens in the political sphere. That is a moving target,” she says. “That is beyond us.”
Deep Dive
Biotechnology and health
How scientists traced a mysterious covid case back to six toilets
When wastewater surveillance turns into a hunt for a single infected individual, the ethics get tricky.
An AI-driven “factory of drugs” claims to have hit a big milestone
Insilico is part of a wave of companies betting on AI as the "next amazing revolution" in biology
The quest to legitimize longevity medicine
Longevity clinics offer a mix of services that largely cater to the wealthy. Now there’s a push to establish their work as a credible medical field.
There is a new most expensive drug in the world. Price tag: $4.25 million
But will the latest gene therapy suffer the curse of the costliest drug?
Stay connected
Get the latest updates from
MIT Technology Review
Discover special offers, top stories, upcoming events, and more.