The Tiny Robots Revolutionizing Eye Surgery
Last September, Robert MacLaren, an ophthalmologist and professor at Oxford University, plunged a tiny robotic arm into William Beaver’s eye. A membrane had recently contracted on the 70-year-old priest’s retina, pinching it into an uneven shape and causing him to see the world as if reflected in a hall of mirrors.
Using a joystick and a camera feed, MacLaren guided the arm of the Robotic Retinal Dissection Device, or R2D2 for short, through a tiny incision in the eye, before lifting the wrinkled membrane, no more than a hundredth of a millimeter thick, from the retina, and reversing Beaver’s vision problems.
It was the first operation performed inside the human eye using a robot. Since September, five more patients have undergone robot-assisted operations at Oxford’s John Radcliffe Hospital in England, including one in which a virus, used in gene therapy to halt the effects of retinal degeneration, was planted on the retina itself, a procedure only made possible by R2D2’s unprecedented precision.
“My movements were improved and finessed by the robot,” MacLaren says. “I could even let go and the robot would hold everything securely in place.”
In the past decade the use of robots in surgery has become commonplace. Da Vinci, an American-made surgical robot that is used to repair heart valves, among other things, has operated on more than three million patients around the world. Robotic surgery provides numerous benefits, offering surgeons a greater degree of control while simultaneously reducing a patient’s trauma and risk of infection. The market for medical robotic systems will exceed $17 billion by 2020, according to some estimates. But until now surgical robots have been too bulky to be used in certain procedures at small scale (da Vinci, for example, is around the size of an elephant, its bulk necessary to push against the forces of the body wall).
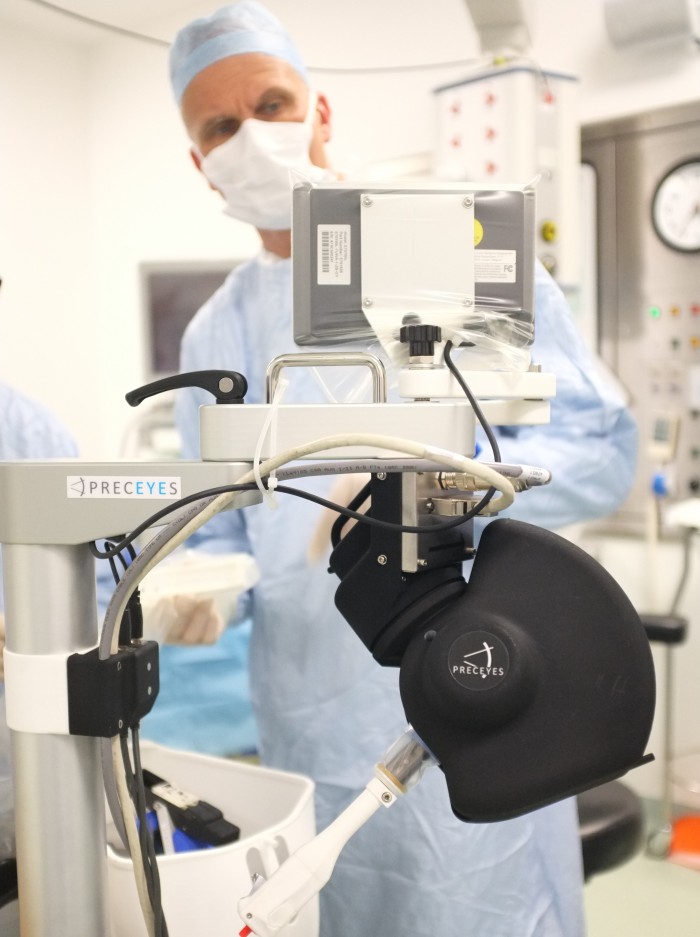
R2D2, which was developed by Preceyes BV, a Dutch medical robotics firm established by the University of Eindhoven, is not the only robot targeting the human eye. Chris Wagner, head of advanced surgical systems at Cambridge Consultants, has led a team in the development of Axsis—one of the smallest known robots for surgical use, its external body is the size of a can of soda.
“Building a surgical robot that can work on the size scale of the lens of an eye, which is less than 10 millimeters across, is difficult,” says Wagner, whose team began work on Axsis last April. For example, the cables that enable the robot to navigate are each 110 microns across, a little over the diameter of a human hair.
Both R2D2, which, according to MacLaren’s estimates, will cost around $1 million, and Axsis are prototype robots currently unavailable on the market. Cambridge Consultants hopes that future versions of its Axsis robot will prove affordable for smaller hospitals, thereby lowering the barrier to entry for less experienced robotic surgeons.
“With this system, we're trying to expand the range of procedures that should be considered candidates for robotic technology, in terms of the size of the manipulations and the size of the access,” says Wagner. He hopes that Axsis could, for example, be used to operate on cataracts, the most commonly performed surgery in developed countries. Oxford’s MacLaren, however, is skeptical of the need for robotic support in this kind of routine eye operation. To meet the demand, “thousands of machines” would have to be manufactured, he says. “It’s clearly not necessary. But these robots do open up a new chapter of operations that are currently impossible.”
MacLaren believes that R2D2 and other robots like it will enable surgeons to, for the first time, operate underneath the retina and interact with blood vessels in the eye. “Undoubtedly this will lead to improvements in quality of eye surgery that require highly technical procedures,” he says. “But most significantly they will open the door to new operations for which the human hand does not have the necessary control and precision.”
Keep Reading
Most Popular
Large language models can do jaw-dropping things. But nobody knows exactly why.
And that's a problem. Figuring it out is one of the biggest scientific puzzles of our time and a crucial step towards controlling more powerful future models.
How scientists traced a mysterious covid case back to six toilets
When wastewater surveillance turns into a hunt for a single infected individual, the ethics get tricky.
The problem with plug-in hybrids? Their drivers.
Plug-in hybrids are often sold as a transition to EVs, but new data from Europe shows we’re still underestimating the emissions they produce.
Google DeepMind’s new generative model makes Super Mario–like games from scratch
Genie learns how to control games by watching hours and hours of video. It could help train next-gen robots too.
Stay connected
Get the latest updates from
MIT Technology Review
Discover special offers, top stories, upcoming events, and more.