Injectable Wires for Fixing the Brain

In a basement laboratory at Harvard University, a few strands of thin wire mesh are undulating at the bottom of a cup of water, as if in a minuscule ribbon dance. The meshes—about the length of a pen cap—are able to do something unprecedented: once injected into the brain of a living mouse, they can safely stimulate individual neurons and measure the cells’ behavior for more than a year.
Electronic brain interfaces like these could someday be crucial for people with neurological diseases such as Parkinson’s. The disease causes a group of neurons in one area of the brain to begin dying off, triggering uncontrollable tremors and shakes. Sending targeted electrical jolts to this area can help whip the living neurons back into shape and stop Parkinson’s symptoms.
Today people can undergo an electrical treatment called deep brain stimulation. But it has big limitations. It involves implanting rigid, dense electrodes in the brain. That’s far from ideal in such a soft organ: after about four weeks, scar tissue begins to build up. The only way to get the electrodes to work through this tissue is to keep upping the voltage used to excite the neurons. That can be dangerous, and sometimes another surgery is required to replace the implant.
Charles Lieber, a Harvard chemist and nanomaterials pioneer, had a different idea: a conductive brain interface that mirrors the fine details of the brain itself. Just as neurons connect with each other in a network that has open spaces where proteins and fluids pass through, the crosshatches in Lieber’s bendable mesh electronics leave room for neurons to fit in, rather than being pushed to the side by a boxy foreign object. “This device effectively blurs the interface between a living system and a non-living system,” says Guosong Hong, a postdoc in Lieber’s lab.
The extremely flexible mesh, made of gold wires sandwiched between layers of a polymer, easily coils into a needle so it can be injected rather than implanted, avoiding a more extensive surgery. Part of the mesh sticks out though the brain and a hole in the skull so that it can be wired up to a computer that controls the electric jolts and measures the neurons’ activity. But eventually, Lieber says, the controls and power supply could be implanted in the body, as they are in today’s systems for deep brain stimulation.
The researchers foresee the mesh having many uses beyond Parkinson’s. It might help treat depression and schizophrenia more precisely than today’s drugs, which bathe the entire brain in chemicals and cause an array of side effects.
First, though, it needs to be tested in humans. Lieber’s group is partnering with doctors at Massachusetts General Hospital and will soon begin experiments in people with epilepsy.


Left: The mesh electronics—lines of gold between layers of a polymer—are produced in batches on a silicon wafer.
Right: This close-up of the mesh shows a pad in the middle that stimulates neurons. Smaller pads measure their activity.


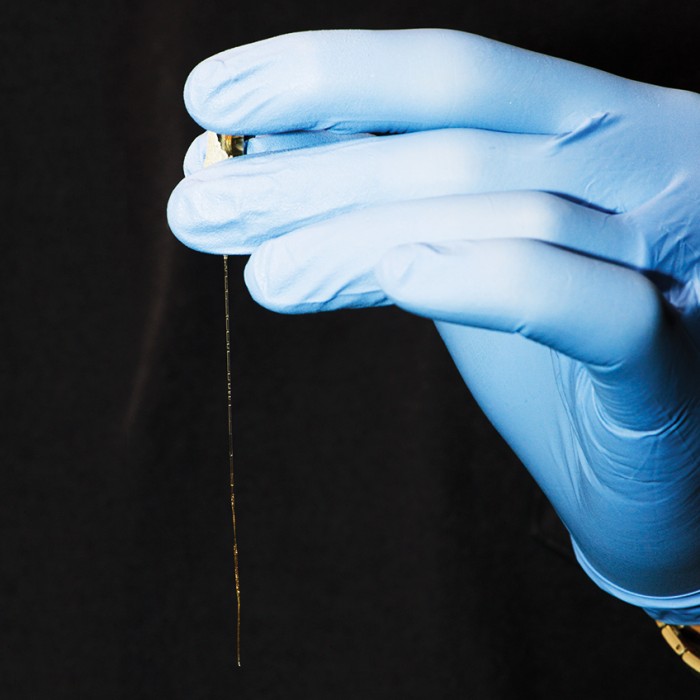
Left: As demonstrated here in water, the mesh is extremely flexible once in the brain.
Right: Out of the brain (or water), the structure goes limp.


Keep Reading
Most Popular
Large language models can do jaw-dropping things. But nobody knows exactly why.
And that's a problem. Figuring it out is one of the biggest scientific puzzles of our time and a crucial step towards controlling more powerful future models.
The problem with plug-in hybrids? Their drivers.
Plug-in hybrids are often sold as a transition to EVs, but new data from Europe shows we’re still underestimating the emissions they produce.
Google DeepMind’s new generative model makes Super Mario–like games from scratch
Genie learns how to control games by watching hours and hours of video. It could help train next-gen robots too.
How scientists traced a mysterious covid case back to six toilets
When wastewater surveillance turns into a hunt for a single infected individual, the ethics get tricky.
Stay connected
Get the latest updates from
MIT Technology Review
Discover special offers, top stories, upcoming events, and more.