Identifying Signs of Chronic Brain Injury in Living Football Players
Eight former pro football players learned this year that they have signs of a degenerative brain disorder called chronic traumatic encephalopathy (CTE), a condition linked to depression, dementia, and memory loss. These somber findings were uncovered using a new method of brain imaging that, for the first time, enables researchers to spot signs of the condition in the living brain. Previously CTE could only be identified after a victim died.
The new method could help quantify the risks of repetitive blows to the head (see “Images of a Hard-Hitting Disease” and “Military Brains Donated for Trauma Research”). It could also help future players avoid the degenerative and sometimes lethal condition by limiting their exposure, and it may help scientists develop better protective gear and treatments.
Starting in 2002, researchers began to identify CTE in the brains of deceased former NFL players. Since then, dozens of former players have been diagnosed with CTE this way. “That work was very interesting and very rewarding, but the problem was you could only get this diagnosis after someone was dead,” says neurosurgeon and former Pittsburgh Steelers physician Julian Bailes. “We have no hope in treating them if we can’t diagnose it in people who are alive.”
About three years ago, Bailes began to hunt for methods that could make that diagnosis in living people. He teamed up with a group of researchers at UCLA led by Gary Small, whose team had developed a brain-scanning technique for identifying signs of Alzheimer’s in the brains of living patients. The researchers adapted that method to image a protein called tau, which has been linked to CTE.
A brain autopsy remains the only way to officially diagnose CTE. Pathologists use special dyes that bind to the tau and other proteins to examine the state of the brain cells, and then look for telltale patterns of CTE.
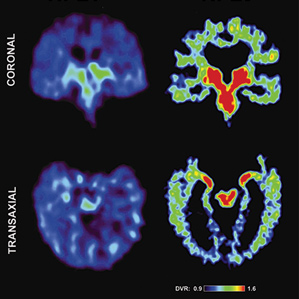
The new method for identifying signs of CTE in living brains is based on a positron emission tomography, or PET scans. The UCLA researchers developed a radioactive compound that can be injected intravenously. The compound circulates through the bloodstream and into the brain, where it gloms onto tau proteins, which can then be measured in a PET scanner. The whole test takes about an hour.
The radioactive compound also sticks to amyloid proteins. Aggregations of both amyloid and tau are considered culprits in Alzheimer’s disease, whereas tau is the main indicator for CTE. Bailes and colleagues say the regions of the brain that are highlighted in PET scans of patients with Alzheimer’s differ from the scans of patients with CTE.
Earlier this year, Bailes and colleagues published the results from five former NFL players; all had accumulations of tau protein in their brains. “For the first time we can see the footprint of prior brain injury, especially the minor and repetitive injuries, and know when there is injury accruing in the brain,” says Bailes.
The UCLA compound is the only PET imaging agent that has been used to detect tau accumulations in living human brains. However, a more specific imaging agent may be on the way—Eli Lilly, which already sells an amyloid-specific PET agent, is currently testing a tau-specific agent.
An advantage of the PET scan method is that it looks at the behavior of living cells, says Bailes. That’s important because CTE-afflicted brains don’t show large structural changes like atrophy, which can show up in other brain scans such as MRIs. “The subtle injury on its surface is not major and life-threatening, but through repetitive hits of this sort, it can cause problems,” says Bailes.
Before the PET scan method can be used for diagnosing CTE, more players and other people need to be scanned to verify it. Some of that additional evidence could come to light soon—the researchers say they are publishing the results of more players in the near future.
The lack of a living diagnosis obscures the true prevalence of CTE in contact sport athletes, military veterans, and the rest of the population. “We don’t know who gets it and why,” says Bailes.
A method for diagnosing CTE in living brains could also help researchers better understand the biological details of the condition, including how it progresses and whether or not it can be reversed. Like autopsy studies, the PET scans show that damaging tau accumulates in regions of the brain that affect memory, behavior, and emotions. There are no specific treatments for CTE, although counseling and medications such as antidepressants may help. Many CTE victims commit suicide, says Bailes. “It’s only by making a diagnosis while they are alive could we think about intervening,” he says.
While the reports of CTE in former NFL players may have football fans concerned about the future of the game, the PET scan method could play a role in protecting athletes and helping the game adapt. A living diagnosis would help researchers develop drugs to treat or prevent CTE. And a better understanding of the injury could perhaps create better helmets to prevent it (See “What’s Next for Concussions in Football”).
If verified, the method could also help athletes, soldiers, and others better assess their risks. “It could very much be a way to screen people, to let them know whether there is a deposition there that indicates they’ve got some kind of injuries,” says Bailes. “Then they could develop strategies for continuing to participate or retire.”
Keep Reading
Most Popular
Large language models can do jaw-dropping things. But nobody knows exactly why.
And that's a problem. Figuring it out is one of the biggest scientific puzzles of our time and a crucial step towards controlling more powerful future models.
How scientists traced a mysterious covid case back to six toilets
When wastewater surveillance turns into a hunt for a single infected individual, the ethics get tricky.
The problem with plug-in hybrids? Their drivers.
Plug-in hybrids are often sold as a transition to EVs, but new data from Europe shows we’re still underestimating the emissions they produce.
Stay connected
Get the latest updates from
MIT Technology Review
Discover special offers, top stories, upcoming events, and more.