System Lets Surgeons Image the Brain While they Operate On It
A new system for visualizing the brain during surgery is helping neurosurgeons more accurately diagnose and treat patients and is even allowing them to perform some procedures that until now have been extremely difficult or even impossible.
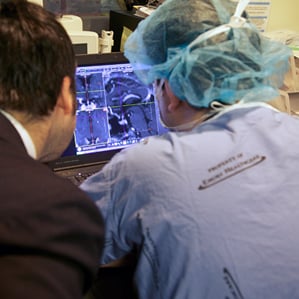
Neurosurgeons can use the imaging technology during surgeries that require small objects—biopsy needles, implants, or tubes to deliver drugs—to be placed at precise locations in the brain. The system provides live magnetic resonance images (MRI) that allow surgeons to monitor their progress during the operation.
Typically, neurosurgeons use an MRI before a surgery to plan the trajectory of the operation, based on the brain’s position relative to a guidance frame that’s screwed onto the patient’s skull, says Robert Gross, a neurosurgeon at Emory University. But the brain can shift before the actual surgery takes place, he says, rendering that MRI inaccurate. To check on what’s happening inside a patient’s skull, doctors have to stop the surgery and perhaps even move the patient out of the operating room.
To address these issues, researchers have been developing new neurosurgical guidance systems that can work with the strong magnets and electronic signals used by MRI scanners. The medical-device company Medtronic, for example, offers a real-time MRI imaging system for neurosurgery. But Gross says the most useful system on the market is offered by MRI Interventions, a medical device company based in Memphis, Tennessee.
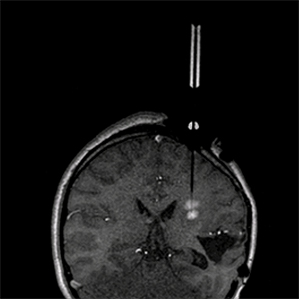
The MRI Interventions system works with conventional MRI scanners. A platform for guiding surgical tools or implants into the brain is affixed to the skull and provides a grid-based system for determining the trajectory. A material in the platform makes the device visible to the MRI scanner. Software from MRI Interventions shows surgeons where their tools are relative to the patient’s brain. That data is displayed on an MRI-compatible monitor to allow surgeons a view of what is happening inside the patient’s skull without interfering with the imaging procedure, which is a problem associated with most electronic equipment.
“If the brain has shifted, you will be able to see that inaccuracy in the trajectory,” says Gross, who uses the system along with medical lasers to destroy small regions of brain tissue that cause seizures in epilepsy patients.
MRI Interventions has installed 25 of its real-time MRI guidance systems: two in Europe and 23 in the United States. Often, neurosurgeons rely on patients to be awake during brain operations so the patients can provide behavioral clues as to whether the surgeon is inserting a tool or treatment device into the intended location. For some procedures, the new technology means that keeping patients awake during the operation is no longer necessary.
Doctors are also using the system to deliver experimental treatments for brain cancer. Researchers at the University of California, San Diego, are using the real-time MRI system to test whether a cancer-killing viral gene therapy can treat malignant brain tumors. “Being able to look at the MRI while the biopsy needle is in the brain makes diagnoses more accurate,” says Santosh Kesari, a neuro-oncologist involved in the gene therapy study. “And when we are trying to deliver treatments, we will know we are getting it to the right place, safely.”
Keep Reading
Most Popular
Large language models can do jaw-dropping things. But nobody knows exactly why.
And that's a problem. Figuring it out is one of the biggest scientific puzzles of our time and a crucial step towards controlling more powerful future models.
How scientists traced a mysterious covid case back to six toilets
When wastewater surveillance turns into a hunt for a single infected individual, the ethics get tricky.
The problem with plug-in hybrids? Their drivers.
Plug-in hybrids are often sold as a transition to EVs, but new data from Europe shows we’re still underestimating the emissions they produce.
Stay connected
Get the latest updates from
MIT Technology Review
Discover special offers, top stories, upcoming events, and more.