Are Surgical Robots Worth It?
Surgical robots allow surgeons to perform a variety of less invasive operations because their miniaturized instruments can work through small incisions in the body and are more dexterous than traditional laparoscopic tools (see “The Slow Rise of the Robot Surgeon”). The result is that patients leave the operating room with a smaller surgical wound with the promise of faster recovery and less scarring.
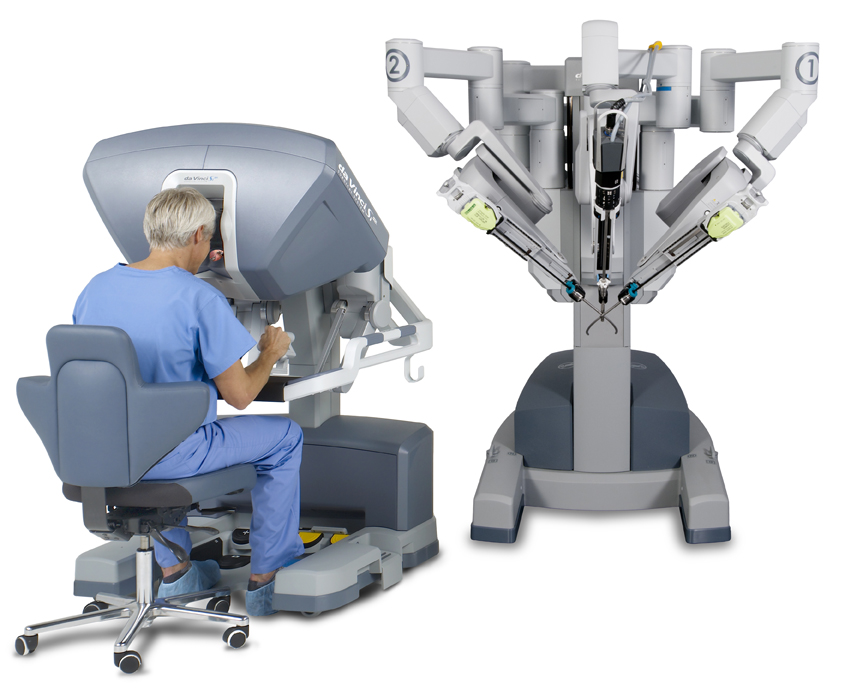
In 2000, Intuitive Surgical’s da Vinci system became the first FDA-approved commercially available robotic surgical platform and has since been used on hundreds of thousands of patients. According to a report on Bloomberg’s news site, the FDA is now taking another look at the system in response to an increase in reports of adverse incidents. As reported by Bloomberg:
What the agency is trying to determine is whether a rise seen in incident reports sent to the agency are “a true reflection of problems” with the robots, or the result of other issues, said Synim Rivers, an [FDA] spokeswoman, in an e-mail. “It is difficult to know why the reports have increased,” she said.
The increase in incidents could be due to the growing number of surgeries performed by the robotic systems, which are not automated but instead driven by a surgeon in a seated at a console. Still, the rise in reports has tripped the wires of the FDA’s Adverse Event Reporting System, so the agency is surveying surgeons on complications they’ve seen and their training, according to Bloomberg.
The systems are quite costly (around $2.5 million) and recent studies suggest they may not provide the improved patient safety that they promise. Researchers reported in the Journal of the American Medical Association last week that robotic-assisted hysterectomies had similar rates of complications to laparoscopic surgeries (which also involves small incisions). The researchers did identify a major difference—the cost of the surgeries. The robotic surgeries cost on average $2,139 more than the laparoscopic procedures.
Image: Intuitive Surgical
Keep Reading
Most Popular
Large language models can do jaw-dropping things. But nobody knows exactly why.
And that's a problem. Figuring it out is one of the biggest scientific puzzles of our time and a crucial step towards controlling more powerful future models.
The problem with plug-in hybrids? Their drivers.
Plug-in hybrids are often sold as a transition to EVs, but new data from Europe shows we’re still underestimating the emissions they produce.
Google DeepMind’s new generative model makes Super Mario–like games from scratch
Genie learns how to control games by watching hours and hours of video. It could help train next-gen robots too.
How scientists traced a mysterious covid case back to six toilets
When wastewater surveillance turns into a hunt for a single infected individual, the ethics get tricky.
Stay connected
Get the latest updates from
MIT Technology Review
Discover special offers, top stories, upcoming events, and more.