Injectable Foam Expands in the Belly, Stops the Bleeding
Two liquids that turn into a solid foam after being injected into the body may one day save the lives of injured soldiers and wounded civilians by slowing internal bleeding so that they can make it to a hospital. The Defense Advanced Research Projects Agency awarded Arsenal Medical a $15.5 million grant in December to further develop the foam technology, which would be delivered to a wounded soldier through the belly button.

Currently, battlefield medics and paramedics have no tools to stop internal bleeding before an injured person reaches a hospital. “The only thing you can do for that is get to the hospital as soon as possible,” says David King, a trauma surgeon at Massachusetts General Hospital and a co-investigator on the foam project. King, who has served as a military doctor in both Iraq and Afghanistan, says death in these military contexts from uncontrolled internal bleeding is a “regular and routine occurrence.”
“Upwards of a quarter of the people who end up dying in combat could potentially have survived,” says Robert Gerhardt, a physician-scientist at the U.S. Army Institute of Surgical Research at Fort Sam Houston, Texas, who is not involved with the foam project. “We can tie a tourniquet around an arm or leg, but when we get to parts of the body that are not accessible—the abdomen, chest, and to some extent within the head—these are areas of the body we can’t get to directly unless we have a surgeon to open them up, find the bleeding vessel, and clamp it,” he says.
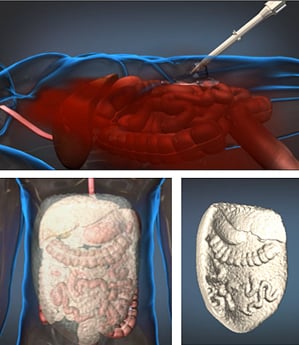
To address this issue, Arsenal Medical in Watertown, Massachusetts, has designed a substance that fills the abdominal cavity and forms a solid foam that can slow internal bleeding. It starts with two liquids. “Mixing those two liquid components causes a chemical reaction that drives the material throughout the abdominal cavity,” says Upma Sharma, head of the foam-technology research at Arsenal. The idea is that the foam would put enough pressure on the site of the injury to slow bleeding for up to three hours so that the soldier could be transported to a hospital. There, a surgeon would remove the block of foam and tend to the soldier’s wounds.
A field medic would inject the two liquids through the injured soldier’s belly button—”a very easy location to find and a safe place to access the cavity,” says Sharma. “You aren’t going to puncture the aorta there,” she says.
The company tested more than 1,200 different mixtures before finding the combination with the right material properties. The foam can’t form too fast or too slow, can’t be too hard or too soft when it’s solid, and surgeons must be able to remove it without doing more damage to the soldier.
One property of Arsenal’s foam that sets its material apart from other attempts to solve the problem is how it interacts with blood, says Sharma. “When we started, we thought you wanted something that would mix well with the blood because that would help it get to the site [of bleeding],” she says. “It turns out that’s not right; you want something that doesn’t mix with blood and instead pushes it out of the way.”
The hardened foam is a polyurethane, a family of materials that is already used in bone cement, vascular grafts, and other medical situations, as well as car seats and insulation.
The team is testing the foam in pigs that are subjected to an internal injury that cuts the liver and a large vein. With the treatment, nearly three-quarters are still alive three hours later.
The team is now monitoring pigs for long-term effects after the foam is removed. The company plans to begin working with the U.S. Food and Drug Administration this year to determine how to test the technology on the battlefield.
A variety of injuries can cause uncontrolled internal bleeding, and the foam technology won’t help everyone. “I don’t think there is going to be a single solution to this,” says Gerhardt.
But for many internal injuries, being able to inject something into the belly is a potential solution, and “an hour or two of additional time may very well make a difference,” he says.
Keep Reading
Most Popular
Large language models can do jaw-dropping things. But nobody knows exactly why.
And that's a problem. Figuring it out is one of the biggest scientific puzzles of our time and a crucial step towards controlling more powerful future models.
The problem with plug-in hybrids? Their drivers.
Plug-in hybrids are often sold as a transition to EVs, but new data from Europe shows we’re still underestimating the emissions they produce.
Google DeepMind’s new generative model makes Super Mario–like games from scratch
Genie learns how to control games by watching hours and hours of video. It could help train next-gen robots too.
How scientists traced a mysterious covid case back to six toilets
When wastewater surveillance turns into a hunt for a single infected individual, the ethics get tricky.
Stay connected
Get the latest updates from
MIT Technology Review
Discover special offers, top stories, upcoming events, and more.