Vision-Restoring Implants That Fit Inside the Eye
A coming generation of retinal implants that fit entirely inside the eye will use nanoscale electronic components to dramatically improve vision quality for the wearer, according to two research teams developing such devices.
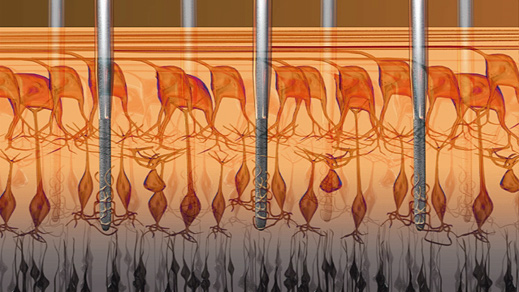
Current retinal prostheses, such as Second Sight’s Argus II, restore only limited and fuzzy vision to individuals blinded by degenerative eye disease. Wearers can typically distinguish light from dark and make out shapes and outlines of objects, but not much more.
The Argus II, the first “bionic eye” to reach commercial markets, contains an array of 60 electrodes, akin to 60 pixels, that are implanted behind the retina to stimulate the remaining healthy cells. The implant is connected to a camera, worn on the side of the head, that relays a video feed.
A similar implant, made by Bionic Vision Australia, incorporates just 24 electrodes. With so few electrodes, the amount of visual information transmitted to the brain is limited: text, for example, is difficult to read. Second Sight recently announced a method by which Argus II wearers are able to visualize Braille instead of traditional text.
Recognizing this limitation, both Second Sight and Bionic Vision Australia have announced that they are developing next-generation devices with 200-plus electrodes. But arrays of nanoscale electrodes, which are currently being incorporated into new retina devices, could someday give blind people 20/20 vision.
“Smaller materials do have the possibility of giving higher-resolution images,” says Shawn Kelly, a bioengineer at Carnegie Mellon University, who is developing a microscale retinal prosthesis. “Smaller electrodes can get closer to individual nerves, and you can have many more of them.”
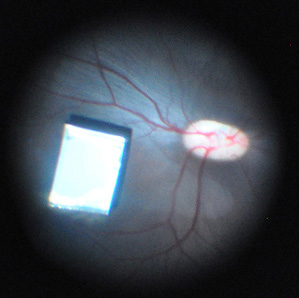
In Israel, a company called Nano Retina has developed an implant that consists of photosensors, circuits, and 676 electrodes, all small enough to fit onto a single implant the size of a child’s fingernail; unlike the Argus II, the device requires no external camera or wires. “The eye is the most confined space in the body,” says Ra’anan Gefen, managing director of Nano Retina. “That’s where miniaturization is needed.”
The company has already tested a prototype in pigs, and it “worked beautifully,” Gefen says. They are now building a human prototype that should improve on both the quality and the number of electrodes, potentially reaching up to 5,000. “Our target is to get to 20/20 [vision],” says Gefen. “I’m sure we can get there.” The company hopes to enter clinical trials within two years.
Another team, this one at the University of California, San Diego, is using nanotechnology to directly mimic cells found in the eye. Massoud Khraiche and colleagues engineered an implant of silicon nanowires that mirror the form, distribution, and function of natural photoreceptors. Uniquely, this approach combines both light detection and neuron stimulation in a single material, with no need for additional photosensors or a camera to capture light.
“Nanowires are perfect for eyes,” says Khraiche. “They capture light well and are tiny.” He presented details on the device at the annual meeting of the Society for Neuroscience in October. The team is currently testing it in rabbits.
“Nanotech implants hold a lot of promise for future applications,” says Kelly, who is not involved with either group, “but they have to be designed carefully.” For one thing, he says, there are safety concerns about applying nanomaterials directly to the retina, and there will need to be ongoing studies about how long a nanotech-derived device can safely survive inside the body.
Keep Reading
Most Popular
Large language models can do jaw-dropping things. But nobody knows exactly why.
And that's a problem. Figuring it out is one of the biggest scientific puzzles of our time and a crucial step towards controlling more powerful future models.
The problem with plug-in hybrids? Their drivers.
Plug-in hybrids are often sold as a transition to EVs, but new data from Europe shows we’re still underestimating the emissions they produce.
Google DeepMind’s new generative model makes Super Mario–like games from scratch
Genie learns how to control games by watching hours and hours of video. It could help train next-gen robots too.
How scientists traced a mysterious covid case back to six toilets
When wastewater surveillance turns into a hunt for a single infected individual, the ethics get tricky.
Stay connected
Get the latest updates from
MIT Technology Review
Discover special offers, top stories, upcoming events, and more.