Gene-Silencing Technique Targets Scarring
A clinical trial of a gene-silencing treatment for reducing excessive scarring is now underway, bringing the number of active clinical trials for the as-yet-unproven gene-silencing process known as RNA interference to nearly 20.
Massachusetts-based RXi Pharmaceuticals has developed a chemically modified version of the small interfering RNAs that drive the biochemical process of RNA interference, or RNAi.
RNAi was discovered in 1998 and has since exploded as a research tool for turning off genes of choice in lab settings. Soon thereafter, biotech and pharmaceutical companies turned their attention to siRNAs—short pieces of RNA, DNA’s cousin, that can prevent the activity of the specific gene they complement—as a potential therapeutic tool, but so far no one has successfully commercialized the technology. The technology holds the potential to reduce the effects of almost any gene in a human cell, if only the interfering RNAs can get inside.
“Because RNA does not normally pass through the membrane of the cell, that delivery step is a major challenge,” says Phil Sharp, a molecular biologist at MIT and a cofounder of an RNAi company called Alynylam (Sharp previously discussed the therapeutic potential of RNAi with Technology Review). Researchers must also strike a balance between the potency of the therapy in targeted cells and side-effects in other cells, he says.
A skin treatment reduces some of the delivery challenge because the target area is easily accessible. RXi injects its scar therapy directly under the outermost layers of the skin, delivering a large amount of the treatment to the target area, thereby reducing the risk of side effects to other parts of the body.
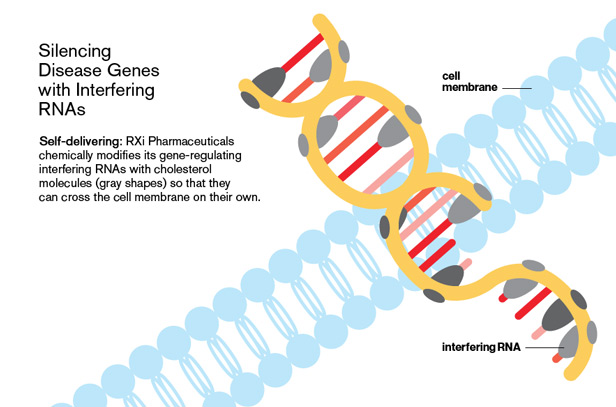
On a molecular level, the company modifies its interfering RNAs so that they are absorbed by the membrane of a cell. The company adds cholesterol molecules, which are normal components of cell membranes, to the RNAs so that the molecule will be more readily absorbed. Once in the membrane, the cholesterol breaks from the RNA molecule, which can then enter the cell body. RXi’s version of siRNAs are also shorter than conventional siRNAs and have been chemically modified to resist the enzymatic wear and tear inside cells.
The scar-treating compound was designed to reduce the expression of a protein called connective tissue growth factor, or CTGF, which regulates several biological pathways involved in wound healing and scar formation. The protein drives production of collagen and other cellular support molecules referred to as matrix proteins.
In some people, CTGF overproduces these components, resulting in excessive scarring such as raised scars or larges scars called keloids. RXi’s CEO Geert Cauwenbergh says the company’s interfering RNA reduces scaring while still allowing CTGF to perform its wound-healing properties. “The interfering RNA doesn’t silence [CTGF] 100 percent—it continues to have some effect, but it’s not excessive,” he says.
RXi has shown that its compound can reduce the amount of CTGF in cultured human cells. Cauwenbergh says that the compound has a beneficial effect on scarring in rats, and that the results of a monkey study should be available in the coming weeks. In theory, the treatment could also benefit any patient hoping to avoid a large normal scar, say from a surgical incision, but RXi has not yet tested this idea.
CTGF already has the attention of Pfizer, which recently acquired a company developing another gene-silencing technique to reduce its effects. However, there are no proven drugs to prevent scar formation, and while people who develop excessive scarring can have the scars surgically removed, they risk another perhaps larger scar forming in its place. “The number of people who will be able to undergo scar remodeling surgery will go up dramatically if this drug works,” says Cauwenbergh.
Keep Reading
Most Popular
Large language models can do jaw-dropping things. But nobody knows exactly why.
And that's a problem. Figuring it out is one of the biggest scientific puzzles of our time and a crucial step towards controlling more powerful future models.
How scientists traced a mysterious covid case back to six toilets
When wastewater surveillance turns into a hunt for a single infected individual, the ethics get tricky.
The problem with plug-in hybrids? Their drivers.
Plug-in hybrids are often sold as a transition to EVs, but new data from Europe shows we’re still underestimating the emissions they produce.
Stay connected
Get the latest updates from
MIT Technology Review
Discover special offers, top stories, upcoming events, and more.