Building Better Implants
Most orthopedic implants–artificial devices like hip and knee joints–last from ten to fifteen years, which means that many patients require several surgeries to replace the parts during their lifetime. Now scientists at Brown University have started working on superior implants that may be easier to monitor and better able to integrate with the surrounding cells of the body.
The researchers, led by associate professor of engineering Thomas Webster, are searching for an easier way to determine whether an implant is successfully integrating with the cells around it. “We wanted to get out of the mode of thinking that the success of an implant could only be seen with an x-ray or a bone scan,” he says.
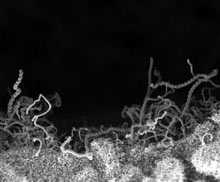
In their search to transform implants into intelligent biosensing surfaces, the team started with titanium, the most popular implant material due to its durability and biocompatibility. The researchers chemically treated the metal and applied an electrical current to it, creating tiny pits on the titanium’s surface. Carbon nanotubes were grown in each pit, where they sprouted like tiny antennae growing up from the metal. Human cells were then applied to the implants. By looking at the amount of electricity that flowed between the nanotubes, the researchers were able to discern what was growing on the surface of the implant: bone, inflammatory scar tissue, or dangerous bacterial biofilm.
“Not only did the nanotubes serve as sensors, but they also promoted bone growth, and we didn’t expect to see that at all,” says Webster. In fact, the bone grown using the implants with carbon nanotubes grew twice as fast as, and contained more calcium than, bone grown on implants without the antennae. It’s important for bone to meld with the implant in order for it to work well.
Webster says that there are several possible explanations for the bone growth. Because bone is nanofibrous, the carbon nanotubes may have mimicked the way that collagen grows. Or perhaps the electricity conducted between the tubes stimulated the cells around them to grow faster. The third possible reason for the cells’ stimulated growth may be in the unique surface energetics created by the nanomaterial.
Whatever the reason for the increased bone growth, the results of this research, published in a recent issue of the journal Nanotechnology, are promising. Webster says that his team is working on the next step for intelligent implants, which is to create devices that not only detect how bone is growing around them, but also react to medical problems. He says that with future implants, doctors may be able to fill the carbon nanotubes with different drugs to be released at specific times. For example, if the device senses that a film of bacteria is growing over the implant, a doctor can release antibacterial drugs directly into the infection. Doctors could also use the tubes to release other drugs, from anti-inflammatory medications to bone-building agents.
Other researchers are enthusiastic about the device, although concerns about safety remain. “Carbon nanotubes as such are not biodegradable,” says Cato Laurencin, a professor of biomedical and chemical engineering at the University of Virginia. “Also, there are conflicting reports in the literature about the safety of carbon nanotubes for human use. Some believe the conflicts are due to preparation techniques.” Scientists are still unsure, Laurencin says, of how nanotubes are flushed out of the body.
Next year, Webster’s team plans to test its orthopedic devices in animals to see if they achieve the same results. “This field has a long way to go to create really intelligent implants, but we are going to get there,” he says.
Keep Reading
Most Popular
Large language models can do jaw-dropping things. But nobody knows exactly why.
And that's a problem. Figuring it out is one of the biggest scientific puzzles of our time and a crucial step towards controlling more powerful future models.
The problem with plug-in hybrids? Their drivers.
Plug-in hybrids are often sold as a transition to EVs, but new data from Europe shows we’re still underestimating the emissions they produce.
How scientists traced a mysterious covid case back to six toilets
When wastewater surveillance turns into a hunt for a single infected individual, the ethics get tricky.
Google DeepMind’s new generative model makes Super Mario–like games from scratch
Genie learns how to control games by watching hours and hours of video. It could help train next-gen robots too.
Stay connected
Get the latest updates from
MIT Technology Review
Discover special offers, top stories, upcoming events, and more.