Fake Skin Kills Bacteria
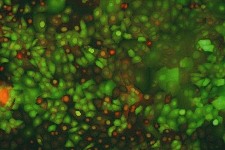
One of the problems with artificial skin is its vulnerability to infection. Synthetic skin is used in burn treatment and plastic surgery, but blood vessels, which carry the immune system’s machinery, may not connect to the new dermis for a week or two. “Without blood vessels, bacteria can grow and cause infection,” says Ioannis Yannas, a bioengineer and materials scientist at MIT who helped develop the first artificial-skin product, approved by the U.S. Food and Drug Administration in the mid-1990s. In a new approach, cultured skin cells are genetically modified to produce higher levels of an antibacterial protein. The cells multiply in the lab and are injected into a collagen matrix of artificial skin. “We’re using genetic modification to try to get the cultured skin to behave more like normal skin,” says Dorothy Supp, a researcher at the Cincinnati Shriners Hospital for Children in Ohio, who led the project. Supp cautions that the engineered cells are far from clinical use: the true test of their bacteria-fighting properties will come in the complex environment of a real wound. The researchers are planning experiments in animal models. The technique could eventually be used to make skin that can sweat and tan after implantation.
Keep Reading
Most Popular
Large language models can do jaw-dropping things. But nobody knows exactly why.
And that's a problem. Figuring it out is one of the biggest scientific puzzles of our time and a crucial step towards controlling more powerful future models.
The problem with plug-in hybrids? Their drivers.
Plug-in hybrids are often sold as a transition to EVs, but new data from Europe shows we’re still underestimating the emissions they produce.
Google DeepMind’s new generative model makes Super Mario–like games from scratch
Genie learns how to control games by watching hours and hours of video. It could help train next-gen robots too.
How scientists traced a mysterious covid case back to six toilets
When wastewater surveillance turns into a hunt for a single infected individual, the ethics get tricky.
Stay connected
Get the latest updates from
MIT Technology Review
Discover special offers, top stories, upcoming events, and more.