Covid-19 “long haulers” are organizing online to study themselves

Gina Assaf was running in Washington, DC, on March 19 when she suddenly couldn’t take another step. “I was so out of breath I had to stop,” she says. Five days earlier, she’d hung out with a friend; within days, that friend and their partner had started showing three classic signs of covid-19: fever, cough, and shortness of breath.
Assaf had those symptoms too, and then some. By the second week, which she describes as “the scariest and hardest on my body,” her chest was burning and she was dizzy. Her friend recovered, but Assaf was still “utterly exhausted.” A full month after falling ill, she attempted to go to grocery shopping and ended up in bed for days.
She didn't initially have access to a coronavirus test, and doctors who saw her virtually suggested she was experiencing anxiety, psychosomatic illness, or maybe allergies. “I felt very alone and confused, and doctors had no answers or help for me,” says Assaf, whose symptoms persist to this day.
In those first few months, Assaf found a legion of people in situations similar to her own in a Slack support group for covid-19 patients, including hundreds who self-identified as “long-haulers,” the term most commonly used to describe those who remain sick long after being infected.
There, she noticed, long-haulers were trying to figure themselves out: Did they have similar blood types? Get tested at a certain time? Have a common geographic or demographic denominator?
So Assaf, a technology design consultant, launched a channel called #research-group. A team of 23 people, led by six scientists and survey designers, began aggregating questions in a Google form. In April, they shared it within the Slack group and on other social-media groups for long-haulers like them.
In May, this group, which now calls itself Patient-Led Research for Covid-19, released its first report. Based on 640 responses, it provides perhaps the most in-depth look at long-haulers to date and offers a window into what life is like for certain coronavirus patients who are taking longer—much longer—to recover.
Until recently, the idea that a person could have the coronavirus for a long time was foreign. Doctors still don’t know what to do with these patients. At the beginning of the pandemic, those who got sick followed one of two paths: either they recovered or they died. Long-haulers don’t fit in either bucket.
The existence of a third path is only now being acknowledged. It wasn’t until late July that the US Centers for Disease Control published a paper recognizing that as many as one-third of coronavirus patients not sick enough to be admitted to the hospital don’t fully recover.
Zijian Chen, the medical director at Mount Sinai’s Center for Post-Covid Care in New York, says he and his colleagues noticed by late April that some patients weren’t recovering. “That is when we realized that patients will need further care,” he says.
What that care entails, however, remains fuzzy. Part of the problem is there isn’t a definition for what constitutes a long-hauler. Chen says Mount Sinai’s program includes “patients with a positive test result for covid-19 and [whose] symptoms persist for more than one month after the initial infection.”
The Patient-Led Research team’s survey targeted patients who felt symptoms for longer than two weeks; importantly, some respondents who reported symptoms were not able to get tested, which would have disqualified them from Chen’s program. The CDC’s paper was based on interviews with subjects conducted 14 to 21 days after they received a positive test result.
Chen hopes to conduct clinical care and research to better understand long-haulers’ symptoms. But he says it’s difficult to devote time or personnel to the task in the midst of a pandemic.
Susannah Fox, who researches online movements within chronic-disease communities, says patient-led research groups such as the one Assaf started will increasingly command the attention of medical researchers, particularly during crises when doctors and scientists are overwhelmed.
“The future of health care and technology is being built in these patient communities,” she says, noting that many early adopters of online bulletin boards and virtual communities were people with rare or chronic diseases who wanted to meet other people like them.
Today, the Patient-Led Research team has new digital tools at its disposal that allow its members to connect and carry out their own research while isolated at home. One resource in particular—the Slack support group, which was created by a company called Body Politic—has been crucial to the team’s efforts.
When the coronavirus struck New York, Body Politic was an emerging media company based in New York City that aimed to highlight underrepresented voices. Then the pandemic hit. Within days of one another, three Body Politic employees got sick with what they all suspect was the disease. “Our priorities shifted,” says Fiona Lowenstein, founder and editor in chief, who tested positive.
The company’s first support group for covid patients wasn't on Slack, says Sabrina Bleich, Body Politic’s creative director, who was among those to fall ill. The group initially gathered followers on Instagram, but when that became too overwhelming, they started a WhatsApp chat group. Within a couple of days, though, the group had exceeded the WhatsApp group limit of 256. She says Slack “felt like the right option to house a large group of people, be adaptable as we grew, and allow for many different communities and conversation streams to occur simultaneously.”
That Slack group has ballooned to more than 7,000 active members. “There was a huge group of patients who felt alone,” Lowenstein says. “They had no idea that they were not alone.”
There are subgroups based on geography (“The UK group is very active,” Lowenstein says) and symptoms (neurological symptoms are a popular topic). Members are from all over the world, though Lowenstein suspects the fact that it’s on Slack might bias its participation toward those who know how to use the software.
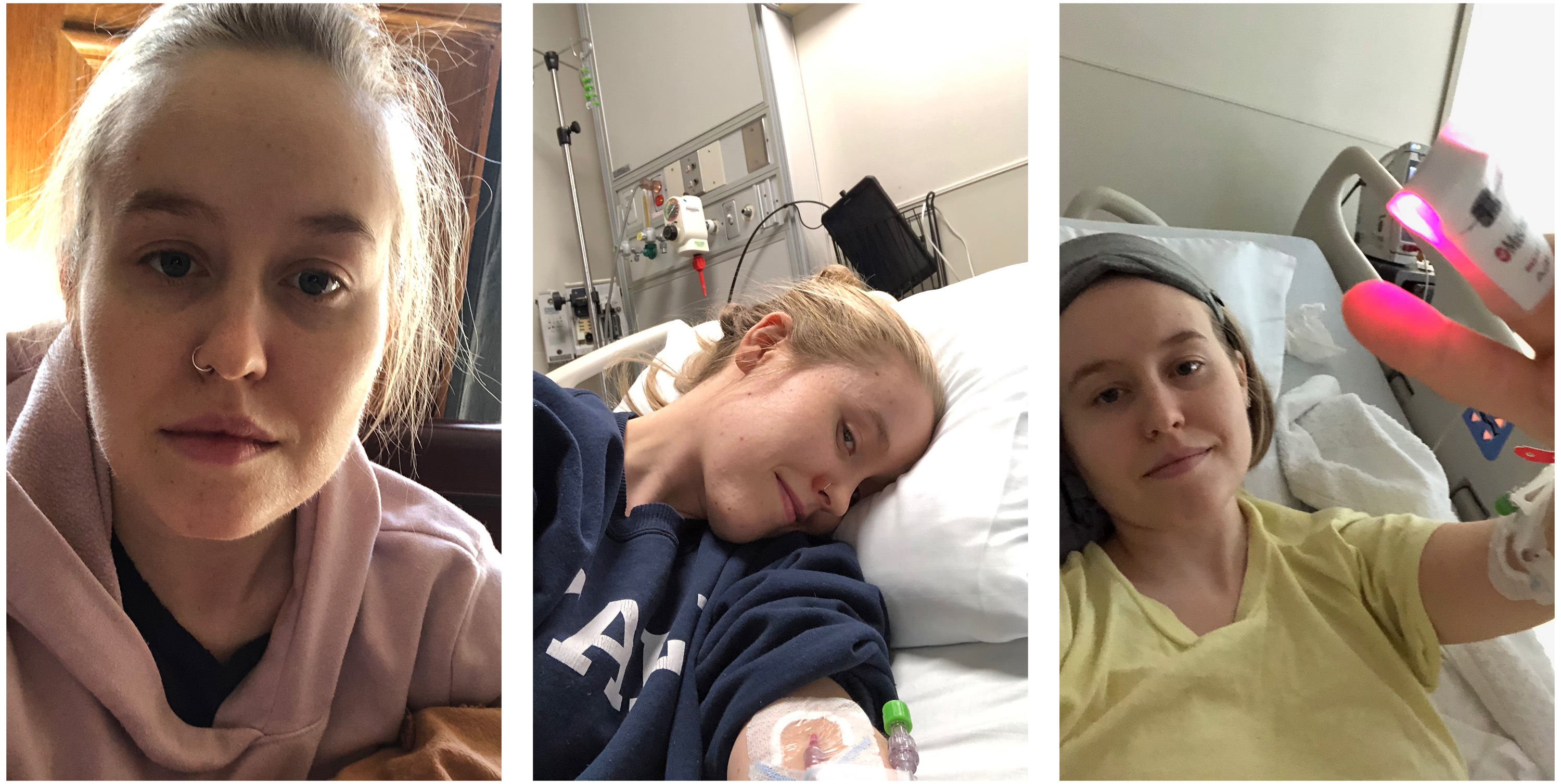
Despite its limits, the Slack group allowed the coronavirus long-haulers in the Patient-Led Research group to find one another. It made it possible for them to coordinate their efforts and launch a study of their own symptoms. For many, the group has both provided a way to draw medical attention to their condition and served as a form of community during months of quarantine.
The organizers—mostly millennial women—have bonded through working together on this project. Assaf leads the group. Hannah Wei, a qualitative researcher based in Canada, handles qualitative analysis; Lisa McCorkell, a policy analyst in California, has taken on data analysis; and Athena Akrami, a neuroscientist in London, provides statistical analysis. They can all name the exact moment when symptoms set in and precisely what day and time they got worse or better.
Hannah Davis, who handled data analysis and visualization, remembers when she realized she was sick. It was March 25, and she was struggling to read a text message. “We were trying to arrange a video call with a friend, but I couldn’t understand what it was saying,” she says.
She soon developed a persistent low fever and began having difficulty breathing—symptoms typical of the coronavirus. She was told to stay home and was unable to get a test. But Davis calls those issues “mild” compared with those that came later. She had a hard time reading and started to notice phantom smells. She had gastrointestinal issues, and after 103 days she developed a skin rash characteristic of covid-19.
Davis felt isolated. At the time, she was stuck in her Brooklyn apartment—alone, sick, and wishing she could connect with someone who understood what she was going through. The Body Politic Slack group was “a lifesaver,” she says. “I don’t know I could have [kept going] without it.”
When I spoke to her 135 days after she initially fell ill, Davis was still sick, with daily fevers, joint pain, cognitive issues, and more. But she feels a renewed sense of purpose thanks to the Patient-Led Research team.
Many in the group were doing their own research even before they joined forces. Wei, a long-hauler who was diagnosed by X-ray and tested negative 40 days later, was frustrated at the lack of information and resources available for people like her. So she created covidhomecare.ca, which includes Google Doc templates for tracking symptoms (and a log of her own symptoms as a guide).
Wei’s expertise in survey design helped the Patient-Led Research group figure out the best way to go about studying themselves. She notes that the group’s survey results are biased—72% of respondents in the first survey are American, and the respondents are predominantly English-speaking. Seventy-six percent of respondents are white, and most are cisgender females.
Akrami, who gets noticeably breathless as she speaks, ran a statistical analysis to help the group interpret its results. “We asked about 62 different symptoms,” she says. “We invited people who have been tested or not tested and asked if they were negative or positive, then compared the symptoms.”
They found that 60 of those symptoms were as likely to show up in long-haulers who tested positive as those who were tested negative, or never tested for the coronavirus. This result seems to indicate that official tallies of cases may be overlooking a large number of patients.
McCorkell, a long-hauler who tested negative, says that nearly half of survey respondents—all of whom have self-reported coronavirus symptoms—were never tested either.
Of those who were eventually tested, many were found negative but still believe they have the virus, on the basis of their own symptoms or a physician’s diagnosis. False negatives are common in coronavirus testing, particularly for people who are tested too soon or too long after being infected.
Still, the survey captured data particular to how long-haul patients experience the disease and its symptoms. “Even when controlling for the time of test, the only difference in symptoms between those who tested positive and those who tested negative is that those who tested positive reported loss of smell and loss of taste more often,” says McCorkell.
The timing of certain symptoms among long-haulers also seems to fluctuate in a kind of pattern. According to the survey, neurological and gastrointestinal symptoms tend to appear around the second week, then dip, and then rise again around the third or fourth month.
Davis was grateful when a fellow long-hauler warned her that days 90 through 120 were the hardest. “It’s crowdsourced recovery,” she says. The survey’s results suggest that neurological symptoms are common for long-haulers: nearly two-thirds of patients described debilitating dizziness, while blurry vision, trouble concentrating, and “brain fog” were also cited frequently. More than a fifth of patients described memory loss and hallucinations.
McCorkell says that with the next survey, due out in the next few weeks, the group will attempt to reach more respondents from Black, Hispanic/Latino, and indigenous communities—groups that have been hit hardest by the coronavirus. And Akrami hopes she can pull in the bigger Body Politic community to help translate survey results into other languages and disseminate the information.
But the long-haulers are now outgrowing their own group. Davis says the Patient-Led Research team is raising money to pay for more Slack users as their numbers grow. “I was lucky to have this experience that I hope is accessible for all long-haulers,” she says. Within the group, “it’s singularly most people’s resource for medical guidance.”
During a time of extreme isolation and uncertainty, Davis and the other organizers are grateful for their Slack group, and to have found each other. “This support group has been one of the biggest gifts of my life,” she says.
Deep Dive
Humans and technology
Building a more reliable supply chain
Rapidly advancing technologies are building the modern supply chain, making transparent, collaborative, and data-driven systems a reality.
Building a data-driven health-care ecosystem
Harnessing data to improve the equity, affordability, and quality of the health care system.
Let’s not make the same mistakes with AI that we made with social media
Social media’s unregulated evolution over the past decade holds a lot of lessons that apply directly to AI companies and technologies.
Stay connected
Get the latest updates from
MIT Technology Review
Discover special offers, top stories, upcoming events, and more.