Gene sleuths are tracking the coronavirus outbreak as it happens
In the unprecedented outbreak of a new coronavirus sweeping the world, the germ’s genetic material may ultimately tell the story not just of where it came from, but of how it spread and how efforts to contain it failed.
By tracking mutations to the virus as it spreads, scientists are creating a family tree in nearly real time, which they say can help pinpoint how the infection is hopping between countries.
When scientists in Brazil confirmed that country’s first case of coronavirus late in February, they were quick to sequence the germ’s genetic code and compare it with over 150 sequences already posted online, many from China.
The patient, a 61-year-old from São Paulo, had traveled in Italy’s northern Lombardy region that month, so Italy was likely where he acquired the infection. But the sequence of his virus suggested a more complex story, linking his illness back to a sick passenger from China and an outbreak in Germany.
More on coronavirus
Our most essential coverage of covid-19 is free, including:
How does the coronavirus work?
What are the potential treatments?
What's the right way to do social distancing?
Other frequently asked questions about coronavirus
---
Newsletter: Coronavirus Tech Report
Zoom show: Radio Corona
See also:
Please click here to subscribe and support our non-profit journalism.
As a virus spreads, it mutates, developing random changes in single genetic letters in its genome. By tracking those changes, scientists can trace its evolution and learn which cases are most closely related. The latest maps already show dozens of branching events.
The data is being tracked on a website called Nextstrain, an open-source effort to “harness the scientific and public health potential of pathogen genome data.” Because scientists are posting data so quickly, this is the first outbreak in which a germ’s evolution and spread have been tracked in so much detail, and almost in real time.
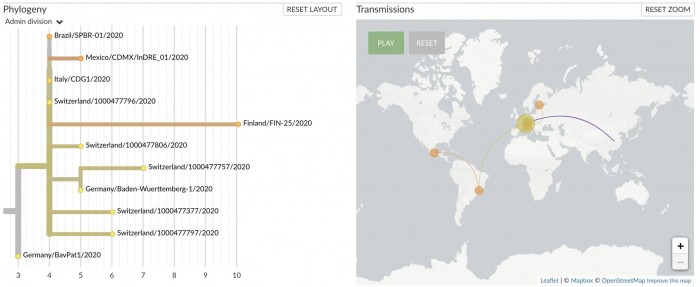
The work of the genome sleuths is helping show where containment measures have failed. It also makes clear that countries have faced multiple introductions of the virus, not just one. Eventually, genetic data could pinpoint the original source of the outbreak.
In Brazil, researchers were able to use gene data to show that its first case, and a second one found later, were not very closely related, says Nuno Faria at the University of Oxford. Samples of the virus from the two patients had enough differences to indicate that they must have been acquired in different locations.
“When combined with the patient travel information, this indicates that the two confirmed cases in Brazil are the result of separate introductions to the country,” Faria wrote in a discussion of his findings.

Since there is no vaccine, experts say the best chance of stopping the virus is through aggressive public health measures, like finding and isolating people who’ve been exposed.
And that’s where the virus’s evolutionary tree is useful, helping to trace the spread of the germ and detect where containment is and isn’t working.
The genetic data shows that the virus entered Europe multiple times. It also now suggests that an outbreak in Munich in January, which researchers believed was caught early, might not have been successfully contained.
Since February 1, about a fourth of new infections—in Mexico, Finland, Scotland, and Italy as well as the first case in Brazil—appeared genetically similar to the Munich cluster, says Trevor Bedford, a researcher at the Fred Hutchinson Cancer Research Center and one of the creators of Nextstrain.
“Patient 1” of the Munich branch was a 33-year-old German businessman from Bavaria who became sick with a sore throat and chills on January 24. Investigators say before feeling ill he'd met with a Chinese business partner visiting from Shanghai, who herself later tested positive for the virus.
Within four days, more employees of the company, Webasto, tested positive. Although the company closed its headquarters, it wasn’t enough. According to the genetic data, the Munich event could be linked to a decent part of the overall European outbreak, which includes more than 3,000 cases in Italy.
“An extremely important take home message here is that just because a cluster has been identified and ‘contained’ doesn’t actually mean this case did not seed a transmission chain that went undetected until it grew to be [a] sizable outbreak,” Bedford posted to Twitter.
That’s exactly what viral detectives think may have happened in Washington State in the US, where a first case was discovered nearly six weeks ago. In February, though, when they sequenced the virus from a new case, they found it shared a specific mutation with the first one.
That meant the two were related and the virus had been silently spreading inside the US all along. Since then, Washington has reported 27 cases and nine deaths, including people who died earlier without being properly diagnosed.
In the wake of the Washington outbreak, critics have blamed the US Centers for Disease Control and Prevention for limiting who could get tested, effectively blinding experts to the course of the outbreak.
Deep Dive
Biotechnology and health
How scientists traced a mysterious covid case back to six toilets
When wastewater surveillance turns into a hunt for a single infected individual, the ethics get tricky.
An AI-driven “factory of drugs” claims to have hit a big milestone
Insilico is part of a wave of companies betting on AI as the "next amazing revolution" in biology
The quest to legitimize longevity medicine
Longevity clinics offer a mix of services that largely cater to the wealthy. Now there’s a push to establish their work as a credible medical field.
There is a new most expensive drug in the world. Price tag: $4.25 million
But will the latest gene therapy suffer the curse of the costliest drug?
Stay connected
Get the latest updates from
MIT Technology Review
Discover special offers, top stories, upcoming events, and more.