3-D Mammography Shown to Improve Detection of Invasive Breast Cancer
A new 3-D imaging technology that typically isn’t covered by health insurance allows radiologists to detect more cases of invasive breast cancer than traditional mammography, a study has found.
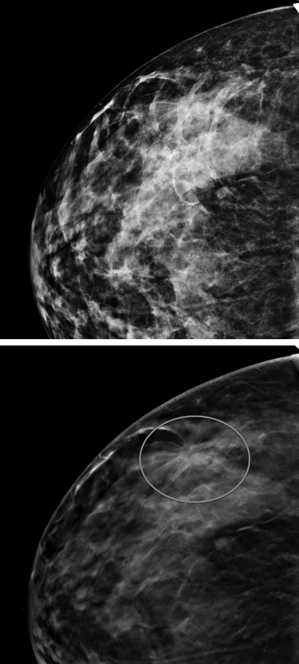
In an analysis of nearly half a million women published in the June 25 issue of the Journal of the American Medical Association, researchers found that 3-D mammography, or tomosynthesis, combined with traditional x-ray screening, was linked to a 41 percent increase in the detection of invasive cancers as well as a 15 percent drop in the recall rate, meaning fewer women were brought back for additional screening because of false alarms.
Daniel Kopans, who founded the breast imaging division at Massachusetts General Hospital and developed tomosynthesis, says the latest evidence could push hospitals to move toward the new screening method.
“Ultimately, radiologists will recognize that if they miss a cancer because they weren’t using tomosynthesis, they could end up being sued by someone who said, ‘Why didn’t you use tomosynthesis? Why did you do my screening as a 2-D mammogram?’” he says.
Currently in the United States, doctors recommend that women over 40 get screened for breast cancer every year, but some researchers argue that the rate of false positives causes patients undue anxiety and creates a burden on the health system. Some medical groups say screening is overused and should instead occur every two years starting at age 50.
Traditional mammography uses side-to-side and top-to-bottom x-rays of the breast. Such 2-D mammograms can create superimposed shadows that look like cancer, and they sometimes fail to detect cancer lesions behind normal tissue. In tomosynthesis, approved by the FDA in 2011, a series of x-ray images are taken in an arc across the breast, resulting in pictures from multiple angles. A computer algorithm then creates a stack of thin layers that a radiologist can read, much like the pages of a book.
The JAMA study was funded by Hologic, which is currently the only company to have an FDA-approved tomosynthesis system in the U.S. (General Electric sells a system in Europe).
The 3-D systems cost about $400,000 to $450,000, compared with about $300,000 for a standard mammography machine, says Rachel Bennett, an analyst at MD Buyline, a research firm specializing in clinical and health-care technology.
Kopans says the cost of the equipment—which works out to around $15 per patient screened—should be weighed against the cost of treating a woman who develops advanced breast cancer, which he says is about $250,000 on average.
Etta Pisano, dean of the College of Medicine at the Medical University of South Carolina, says there still isn’t enough evidence to say whether tomosynthesis should be the standard of care, or even how often women should be screened. “Maybe radiologists should have a mixture of technologies—tomo might just make sense for women with dense breasts,” she says. “I believe we need to move toward more individualized screening.”
Some doctors say 2-D mammography isn’t going to be retired, since it’s better at detecting the tiny calcium deposits that are evidence of ductal carcinoma in situ (DCIS), one of the earliest forms of breast cancer. Instead, the two technologies may be combined. Hologic’s newest scanner, approved by the FDA in 2013, creates both 3-D and 2-D images from the same set of x-rays.
Kopans says the 3-D technology provides a clearer picture of the breast than the 2-D imagery, so radiologists can more accurately analyze the size, shape, and location of any abnormalities and judge whether the tumors are invasive.
“Right now the prohibitive issue is the cost—patients can’t afford to pay for this expensive technology, and there’s no reimbursement to the health-care system,” says Emily Conant, professor and chief of the breast imaging division at the Hospital of the University of Pennsylvania and senior author of the JAMA study. “I think the data supports implementing tomosynthesis for screening, but the financial issue is really tough.”
Keep Reading
Most Popular
Large language models can do jaw-dropping things. But nobody knows exactly why.
And that's a problem. Figuring it out is one of the biggest scientific puzzles of our time and a crucial step towards controlling more powerful future models.
The problem with plug-in hybrids? Their drivers.
Plug-in hybrids are often sold as a transition to EVs, but new data from Europe shows we’re still underestimating the emissions they produce.
Google DeepMind’s new generative model makes Super Mario–like games from scratch
Genie learns how to control games by watching hours and hours of video. It could help train next-gen robots too.
How scientists traced a mysterious covid case back to six toilets
When wastewater surveillance turns into a hunt for a single infected individual, the ethics get tricky.
Stay connected
Get the latest updates from
MIT Technology Review
Discover special offers, top stories, upcoming events, and more.