An Objective Way to Measure Pain
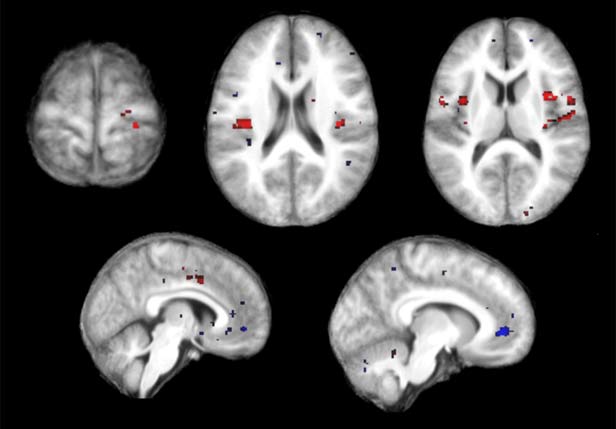
Pain has always been in the eye of the beholder. Doctors evaluating patients, as well as scientists studying pain, have had to rely on subjective descriptions, making pain notoriously difficult to measure and track. A new study from Stanford University takes a first step toward an objective measure for pain.
Researchers found that by pairing functional MRI (fMRI) with a machine-learning algorithm, they could detect specific patterns of brain activity that predicted whether someone was experiencing pain or not. The researchers hope to expand the tool to find brain signatures representing different levels and types of pain, a technology that might one day be useful in clinical practice, drug trials, and pain research.
Scientists have already used fMRI to study the underlying brain structures and patterns of activity involved in pain. But Sean Mackey, a pain researcher and anesthesiologist at Stanford School of Medicine, says that “what we have never done to date is show that you can use that pattern of information to determine whether someone is in pain or not.”
To do that, his team imaged the brain activity of eight people whose skin had been exposed to a heat probe that was modulated to feel either painful or not painful. They used a support vector machine—an algorithm capable of learning and adapting—to analyze the data for patterns of activity common among the subjects.
Researchers have paired brain imaging with pattern-recognition software for more than a decade as a way of decoding brain states or activities—to determine if a subject is performing a particular task or seeing a particular object, for instance.
When the researchers gave the pair of painful and nonpainful heat sensations to 16 new subjects, they found they could separate the two conditions with more than 81 percent accuracy. The research was published online today in PLoS ONE.
Mackey emphasizes that the findings are preliminary. Real-life pain is complex, and this experiment was performed with a small group of subjects in controlled laboratory conditions. But he says the study offers initial evidence that pain, often thought of as entirely subjective, has features that can be measured objectively. “There are some commonalities in these neural signatures from one person to another,” he says.
David Borsook, a pain researcher at McLean Hospital and Harvard Medical School, says that finding an objective measure of pain could radically change how patients are treated. Many scientists have been looking for biomarkers of pain, and Borsook, who was not involved in the study, believes the concept of finding patterns in brain-imaging data “will turn out to be a very robust and useful approach.”
To be useful, such a technique would need to be able to differentiate various types of pain. The Stanford team is evaluating whether the technique can measure chronic pain, rather than a single painful stimulus.
Keep Reading
Most Popular
Large language models can do jaw-dropping things. But nobody knows exactly why.
And that's a problem. Figuring it out is one of the biggest scientific puzzles of our time and a crucial step towards controlling more powerful future models.
The problem with plug-in hybrids? Their drivers.
Plug-in hybrids are often sold as a transition to EVs, but new data from Europe shows we’re still underestimating the emissions they produce.
Google DeepMind’s new generative model makes Super Mario–like games from scratch
Genie learns how to control games by watching hours and hours of video. It could help train next-gen robots too.
How scientists traced a mysterious covid case back to six toilets
When wastewater surveillance turns into a hunt for a single infected individual, the ethics get tricky.
Stay connected
Get the latest updates from
MIT Technology Review
Discover special offers, top stories, upcoming events, and more.